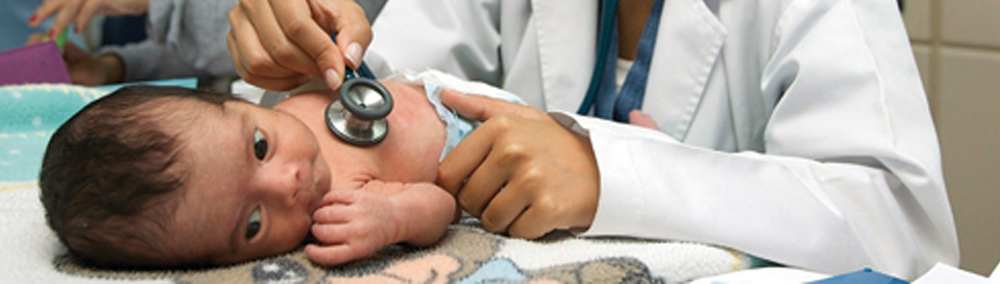
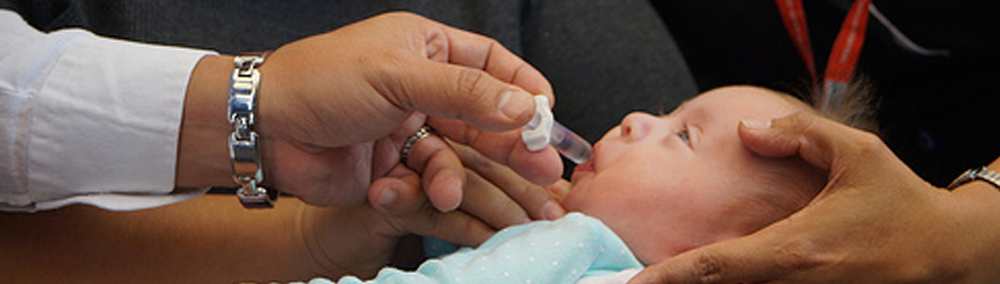
Inequity in health remains one of the most important public health challenges in the Americas, a region that in economic terms is one of the most inequitable in the world. PAHO’s technical cooperation seeks to reduce health inequities through efforts to expand access to health services, advance toward universal health coverage, and address the social determinants of health. A number of lessons have been learned from this work over the past year.
Inequity in health remains one of the most important public health challenges in the Americas, a region that in economic terms is one of the most inequitable in the world. PAHO’s technical cooperation seeks to reduce health inequities through efforts to expand access to health services, advance toward universal health coverage, and address the social determinants of health. A number of lessons have been learned from this work over the past year. Most countries of the Region recognize health as a basic right, and those that have not incorporated this right into their constitutions act in accordance with international treaties or agreements that include the concept of health care as a right. Nevertheless, guaranteeing health care as a right also requires the creation of legal and regulatory frameworks that enable the development of social-protection-oriented health policies and the achievement of universal health coverage. PAHO has a fundamental role in the search for and the promotion of consensus on these important issues and in providing support for addressing the more technical challenges.
It is important to recognize that there is no one-size-fits-all pathway to advancing universal coverage; countries must approach this goal at their own pace and according to their individual needs. In nearly every case, however, efforts to advance universal health coverage have greater impact and sustainability with the inclusion of civil society and the private sector throughout the process.
Social security institutions are important potential partners in the pursuit of universal health coverage. As major health-care providers in many countries, they have valuable insights regarding the development of services and models of care. PAHO can promote effective coordination and productive dialogue between these and other potential partners under the leadership of each country's health authority.
It is also essential to include communities and municipal authorities in underserved or at-risk areas in efforts to advance universal health coverage as well as other health efforts. Collaboration between health authorities and local actors often brings to light challenges and costs of health inequity that would otherwise remain hidden.
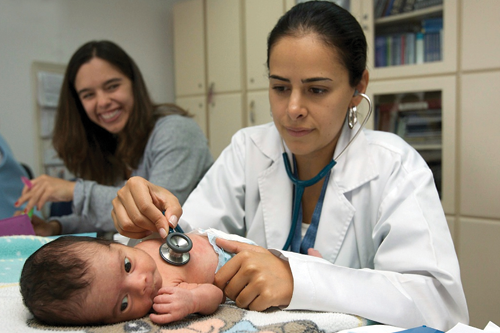 Efforts to increase intersectoral action are fundamental to addressing the social determinants of health and reducing health inequities. This requires engagement and coordination with sectors beyond health and strong advocacy for “health in all policies.” Equally important is strong institutional capacity to marshal evidence on health inequalities as well as on the impact of policies and programs on health equity and the progressive attainment of universal health coverage. Invariably, it will be essential for data—especially those related to social determinants of health—to be disaggregated at the local level to better identify health gaps in vulnerable populations and to develop appropriate interventions.
Efforts to increase intersectoral action are fundamental to addressing the social determinants of health and reducing health inequities. This requires engagement and coordination with sectors beyond health and strong advocacy for “health in all policies.” Equally important is strong institutional capacity to marshal evidence on health inequalities as well as on the impact of policies and programs on health equity and the progressive attainment of universal health coverage. Invariably, it will be essential for data—especially those related to social determinants of health—to be disaggregated at the local level to better identify health gaps in vulnerable populations and to develop appropriate interventions. Strategic partnerships with other actors are increasingly important for PAHO’s work and for advancing health in the Region. The Organization has a long record of partnering successfully with other government sectors—including agriculture and education—as well as with nongovernmental and faith-based organizations, universities, foundations, other development agencies, and communities. PAHO has also been a key facilitator of horizontal cooperation, especially South-South and triangular cooperation to exchange expertise and technologies and to promote, document, and share best practices and lessons learned. Going forward, this work should be strengthened and expanded as a top priority of PAHO’s technical cooperation work.
PAHO’s strategy of country-focused cooperation emphasizes the need to identify and address specific country needs and priorities, to coordinate with other in-country cooperation actors, and to promote sustainability through capacity building and country leadership. Country “ownership” is vital not only to the success of technical cooperation but also to the sustainability of achievements. It requires alignment of technical cooperation programs with established national policies and priorities. Key stakeholders must be involved in the consultation process and implementation as well as in monitoring and data collection. This not only ensures greater “buy-in,” it builds capacity for country leadership.
Lessons from the Health Agenda for the Americas
A mid-term evaluation of the Health Agenda for the Americas 2008–2017 was conducted during 2012 and, after being presented in draft form to the 28th Pan American Sanitary Conference (CSP28/6), was finalized in early 2013 (SPBA7/4). The evaluation was a country-led process involving all 35 PAHO Member States, five subregional integration bodies, and 19 UN and other cooperation agencies.
*Strengthening the national health authority; tackling health determinants; increasing social protection and access to quality health services; diminishing health inequalities among countries and inequities within them; reducing the risk and burden of disease; strengthening the management and development of health workers; harnessing knowledge, science and technology; strengthening health security. |
Human resources capacity must be an overarching consideration for all technical cooperation, as it can facilitate or hinder its success. In the area of NCDs, for example, increased political commitment has not automatically translated into adequate human resources for managing national NCD programs, implementing strategies, or improving quality at the level of patient care. Technical cooperation programming must ensure that countries have strategic human resources plans that are well aligned with projects and programs.
 Partnerships with relevant international organizations and professional associations can help leverage technical assistance and maximize the use of resources—“doing more with less”—which is especially important in light of continuing global economic difficulties. Enhancing coordination between partners can also lead to better results; in many instances, however, the role and responsibilities of PAHO and other partners need to be redefined or adjusted to better address project needs. Joint communication efforts and coordination on priority health issues have led to greater engagement with and participation of various stakeholders and communities.
Partnerships with relevant international organizations and professional associations can help leverage technical assistance and maximize the use of resources—“doing more with less”—which is especially important in light of continuing global economic difficulties. Enhancing coordination between partners can also lead to better results; in many instances, however, the role and responsibilities of PAHO and other partners need to be redefined or adjusted to better address project needs. Joint communication efforts and coordination on priority health issues have led to greater engagement with and participation of various stakeholders and communities. The need for more effective coordination is particularly urgent in the case of emergencies and disasters. Although most countries in the Region now have the capacity to respond to minor or moderate emergencies without international support, responding to major disasters and coordinating massive international assistance remains a significant challenge. Ministries of health should take the lead in establishing coordinating mechanisms in the health sector for receiving and sending international humanitarian assistance. There is also a need for better mechanisms to coordinate the participation of actors in the Health Cluster and ensure adaptability according to national context, ideally through the involvement of fewer and more specialized actors. This would help create synergies among agencies.
 Another important lesson is the critical need to strengthen interprogrammatic work. Regional programs for integrated control of neglected infectious diseases are an example. These have been implemented jointly by programs for immunization, nutrition, childhood diseases (IMCI), tuberculosis, and malaria. Greater interprogrammatic coordination in occupational and environmental health could help to reduce a significant burden of both communicable and noncommunicable diseases.
Another important lesson is the critical need to strengthen interprogrammatic work. Regional programs for integrated control of neglected infectious diseases are an example. These have been implemented jointly by programs for immunization, nutrition, childhood diseases (IMCI), tuberculosis, and malaria. Greater interprogrammatic coordination in occupational and environmental health could help to reduce a significant burden of both communicable and noncommunicable diseases. A continued focus on integrated networks of health services based on primary health care strategies is essential to overcome the continuing segmentation and fragmentation of many countries’ health systems. Together with health systems strengthening and decentralization, integration must remain a cross-cutting priority for the achievement and sustainability of universal health coverage.
An essential part of these efforts is the integration of mental health care into primary care services. This is critical to reducing the large treatment gap for people with mental disorders; more than two-thirds do not receive any care for their condition. At the same time, much work remains to be done to reform psychiatric services and to radically transform the old “asylum” model of hospital-based psychiatric care into a community-based model of care.
Access to evidence-based information to support decision-making continues to be a challenge in many areas of technical cooperation. For example, in the field of disaster risk reduction, evidence on the costs of investment in hospital safety versus the costs of damaged facilities and lost health services is critical for influencing governments, public opinion, and donors. Promoting research for health in other areas remains essential as well, to build the evidence base for policymaking, resource allocation, and the selection of interventions.
Equally important is the development of tools and processes for evaluation and the systematization of technical cooperation experiences to inform programming and policymaking. This is especially true in emerging areas of action that may require new forms of cooperation, often across different disciplines and sectors. For example, a number of initiatives are now under way in the Region that address health inequities through action on the social determinants of health, but these have not been adequately documented or systematized. PAHO can advance this work by helping to measure the impact of health policies, programs, and interventions on the equitable distribution of health gains across different population groups. The resulting evidence can be used to identify new or to adapt existing strategies, policies and programs to more effectively address these issues.
 New communication technologies are already changing the way PAHO provides technical cooperation and have significant potential for creating cost savings and expanding collaboration and reach. Three key PAHO portals—the Regional Platform on Access and Innovation for Health Technology, the Regional Observatory on Human Resources for Health, and the Collaborative Network on Primary Health Care—provide channels for communication and serve as repositories of structured and contextualized information. Virtual meetings can, at lower cost, effectively complement or substitute face-to-face meetings with greater efficiency. However, this change can require a significant cultural shift.
New communication technologies are already changing the way PAHO provides technical cooperation and have significant potential for creating cost savings and expanding collaboration and reach. Three key PAHO portals—the Regional Platform on Access and Innovation for Health Technology, the Regional Observatory on Human Resources for Health, and the Collaborative Network on Primary Health Care—provide channels for communication and serve as repositories of structured and contextualized information. Virtual meetings can, at lower cost, effectively complement or substitute face-to-face meetings with greater efficiency. However, this change can require a significant cultural shift. Increased Internet access and the growing prevalence of mobile devices are expanding audiences for eHealth initiatives and call for continuing innovation in this area. Fully exploiting the potential of new communication technologies for health will also require capacity building—at both the regional and country levels—in the management of new communication tools, new sources of information, and new ways to both collect and share data.
Financial constraints continue to present challenges for both PASB and Member States. This is nowhere clearer than in the pursuit of universal health coverage. Most of the Region’s countries recognize access to health care as a fundamental right, but all struggle to assemble the necessary resources to guarantee this right. Technical cooperation aimed at increasing efficiency in health systems and building capacity in the financing of health systems is as important as efforts to make quality health care more accessible.
Mobilizing financial resources is also critical for preparedness and prevention. Many countries have included disaster risk reduction among their health sector priorities, but they lack resources to make the necessary investments in health infrastructure, essential services, equipment, and training. Engaging the financial sector to strengthen preparedness and prevention, for both disasters and public health more generally, is critical. It is also important to include preparedness and prevention into countries’ development agendas.
 In a context of limited resources, advocacy, communication, and intersectoral collaboration are especially important to help shape opinion and mobilize political support for health. For example, PAHO’s advocacy on neglected infectious diseases led a number of countries to include them in their national health agendas, and a number of donors have shown growing interest in supporting work toward elimination of these diseases. The 2011 UN High-Level Meeting on NCDs, along with global and regional resolutions, has helped mobilize interest and technical changes to improve the quality and effectiveness of NCD programs. Similarly, support from PASB’s new Director has been critical for the all-of-society approach to the elimination of cholera transmission on Hispaniola.
In a context of limited resources, advocacy, communication, and intersectoral collaboration are especially important to help shape opinion and mobilize political support for health. For example, PAHO’s advocacy on neglected infectious diseases led a number of countries to include them in their national health agendas, and a number of donors have shown growing interest in supporting work toward elimination of these diseases. The 2011 UN High-Level Meeting on NCDs, along with global and regional resolutions, has helped mobilize interest and technical changes to improve the quality and effectiveness of NCD programs. Similarly, support from PASB’s new Director has been critical for the all-of-society approach to the elimination of cholera transmission on Hispaniola. Forging strategic alliances with other agencies is essential in this resource constrained environment, for example, among partners such as the Organization of American States, World Bank, and Inter-American Development Bank, among others. A strategic alliance with the OAS’s Inter-American Conference of Ministers of Labor has helped raise the profile of workers’ health on the regional political agenda. Furthermore, the April 2013 San Salvador Declaration on chronic kidney disease from untraditional causes drew attention to this disease that is devastating agricultural communities on Central America’s Pacific Coast. Forging a solution to the problem will require scientists, agricultural communities, and environmental, labor, and agricultural authorities to work together.
Multisectoral action will remain particularly important for technical cooperation and advocacy around NCDs. Involving other sectors, including civil society organizations, is critical to reducing risk factors for NCDs. However, while there are sound examples of collaboration with other sectors, not all have proven sustainable. Efforts to mobilize health partnerships with other sectors could be strengthened by identifying mutual interests that can serve not only health but also other public policy goals.
 In the area of veterinary health, food safety efforts have involved strong collaboration between industry; academia; and the health, agriculture, environment, and consumer sectors. Private-sector support for the Hemispheric Program for the Eradication of Foot-and-Mouth Disease has included essential financing as well as participation in political-strategic decisions that have been key for the sustainability of national programs.
In the area of veterinary health, food safety efforts have involved strong collaboration between industry; academia; and the health, agriculture, environment, and consumer sectors. Private-sector support for the Hemispheric Program for the Eradication of Foot-and-Mouth Disease has included essential financing as well as participation in political-strategic decisions that have been key for the sustainability of national programs. Working with the private sector, while both desirable and essential, requires clear and effective rules of engagement to preempt potential conflicts of interest, both real and perceived. Interdisciplinary consultation and input—from technical cooperation areas as well as legal experts—are an essential part of developing rules of engagement and identifying potential difficulties.
Full implementation of health strategies and policies can be difficult to achieve when these impact the private sector. Industrial interests have mounted strong opposition to regulatory efforts aimed at supporting breastfeeding, regulating marketing and advertising of processed foods, and implementing the provisions of the Framework Convention on Tobacco Control (FCTC). To counteract such opposition, PAHO’s support must include advocacy as well as technical support for legislation.
North-South and South-South collaboration remain valuable ways of promoting and adapting successful public health experience in different countries of the Americas and beyond. Good examples include: agreements between Brazil and Health Canada to strengthen food safety systems and among MERCOSUR countries to address HIV in shared border areas; collaboration among Argentina, the Caribbean Public Health Agency (CARPHA), and PAHO to exchange experiences and strengthen cooperation in areas including noncommunicable diseases, HIV, medicines, transplants, and social determinants of health; and the creation of PAHO Centers of Excellence in countries to promote evidence-based policymaking on the introduction of new vaccines.
 An important value-added of PAHO’s work is the impact that many of its strategies and initiatives have beyond the Region of the Americas. World Immunization Week, held for the second time in 2013, was a global effort inspired by the regional Vaccination Week in the Americas, which celebrated its 11th anniversary in 2013. Other examples include PAHO’s promotion of access to quality medicines and health technologies and the adoption of PAHO technical materials on critical disaster topics in both Member States and in other regions of the world. The wide adoption of the Hospital Safety Index, for example, demonstrates that simple, low-cost tools, if practical and applicable in a range of settings, can enhance participation and stimulate action and investments to save lives around the world.
An important value-added of PAHO’s work is the impact that many of its strategies and initiatives have beyond the Region of the Americas. World Immunization Week, held for the second time in 2013, was a global effort inspired by the regional Vaccination Week in the Americas, which celebrated its 11th anniversary in 2013. Other examples include PAHO’s promotion of access to quality medicines and health technologies and the adoption of PAHO technical materials on critical disaster topics in both Member States and in other regions of the world. The wide adoption of the Hospital Safety Index, for example, demonstrates that simple, low-cost tools, if practical and applicable in a range of settings, can enhance participation and stimulate action and investments to save lives around the world. Going forward, PAHO has a central role to play in ensuring that health authorities and other public health advocates from the Americas contribute effectively to the post 2015 international development agenda. Spaces for dialogue and toolkits such as PAHO’s “Rio+20,” “Health in All Policies,” and “Development Agenda 2015” can be useful for encouraging and guiding countries’ participation in these processes.
The results of regional and global consultations on health in the post 2015 development agenda are also key for PAHO’s own progress going forward. These consultations have produced general agreement on the following points:
- (a) Health must be at the center of sustainable development; it not only contributes to development but is a key outcome and indicator of inclusive, equitable, people-centered, and human-rights–based development. The post-2015 development agenda will require a rigorous framework—different from existing development models—that clearly defines the role of health as well as intersectoral action that supports "health in all policies."
- (b) Countries must redouble efforts to ensure that the Millennium Development Goals are met. Going forward, however, goals must be redrawn and analyzed to reflect sub-national achievements and shortcomings and to stimulate more synergistic approaches to improving conditions for the most vulnerable groups.
- (c) New health priorities must be added to the MDGs that address major contributors to the global and regional burden of disease, particularly noncommunicable diseases and their risk factors, and mental health.
- (d) A core goal that must be included in the new agenda is universal health coverage, understood as access to health for all with quality that addresses social determinants as well as people’s health needs in a human rights framework. Universal coverage must include access to all key interventions, including promotion, prevention, treatment, rehabilitation, and social protection for all. Achieving this people-centered goal requires strong and equitable national health systems that can deliver quality services.
- (e) The overall vision of the post-2015 sustainable development agenda must be centered on human well-being and "living well" and include as a goal maximizing health at all stages of life for every man, woman, and child.
- (f) All this must happen recognizing the need to sustain efforts to prevent and control infectious diseases such as HIV, TB, malaria, and vaccine-preventable diseases.

The challenge will be to keep these concepts and issues—especially universal health coverage and the reduction of health inequities—at the top of the development agenda. This will require active and sustained engagement in future international fora by the countries of the Americas, with PAHO’s full support.
Back to top