

In 2025, the Pan American Health Organization (PAHO) and its Member States made significant progress on critical health priorities while establishing new tools and initiatives to strengthen health systems across the Region.
people died due to suicide in the Americas – and the Region is the only WHO region where suicide mortality has consistently risen over the past two decades.
The Americas face a profound and escalating mental health crisis: 160 million people living with a mental disorder in the Region.
The COVID-19 pandemic intensified these vulnerabilities by disrupting essential services and dramatically increasing demand for care, especially among groups already facing inequities. Structural drivers – including poverty, social inequities, climate-related stressors, and urban violence – continue to strain mental health systems.
In 2025, PAHO officially launched its Regional Suicide Prevention Initiative, aimed at reducing suicide mortality in the Americas with a focus on countries with the highest suicide rates. The initiative was formally launched on 11 September.
The initiative focuses on five strategic areas:
Strengthening multisectoral suicide prevention strategies and action plans
Improving surveillance systems and monitoring of self-harm and suicide
Increasing access to high-quality, person-centered mental health services, integrating digital technologies
Addressing social and environmental risk factors through multisectoral interventions
Increasing public awareness and reducing stigma to improve help-seeking behaviors
Hover over the cards to see more information
Strengthening national suicide prevention strategy and planning/implementation capacity at primary care level
Strengthening community-based surveillance system; operationalizing the National Suicide Prevention Commission; training gatekeepers across all regions to improve early detection, referral, and follow-up support
Scaling state-level suicide prevention by training health workers through the Mental Health Gap Action Programme (mhGAP); conducting national situation analysis to guide priorities and improve surveillance and reporting pathways
PAHO provided extensive technical cooperation to advance mental health legislation across the Region:
Hover over the cards to see more information
Mental health law regulation finalized.
Draft revisions to the mental health law submitted to Congress and currently under review.
First Organic Mental Health Law adopted – aligned with human rights standards.
Mental health law revisions under parliamentary review, deinstitutionalization plan launched; community-based service model established; judicial training on rights completed.
Support provided to draft a new law.
Technical cooperation ongoing for the integration of mental health into primary health care (Argentina, Barbados, Belize, Bolivia [Plurinational State of], Chile, Colombia, Costa Rica, Curaçao, Dominica, Ecuador, Grenada, Guatemala, Guyana, Haiti, Honduras, Mexico, Nicaragua, Panama, Paraguay, Saint Lucia, Suriname, Trinidad and Tobago, Turks and Caicos Islands, Venezuela [Bolivarian Republic of])
Technical cooperation for mental health and psychosocial support responses during Hurricane Melissa
Special Initiative for Mental Health concluded training of over 800 professionals in mhGAP and enabling mental health integration into primary care implementation plans in 20 jurisdictions
Scaled up caregiver skills and parenting training for parents of children with neurodevelopmental disorders nationally, targeting initial support to 36 000 families through a hybrid model
Advanced deinstitutionalization research and expanded mhGAP coverage at primary care level, training 446 professionals and reaching more than 345 000 people
PAHO published a regional analysis on the burden of drug use disorders, providing the most up-to-date epidemiological and policy overview.
Drug use disorders are mental and behavioral disorders resulting from the use of psychoactive substances, characterized by hazardous or harmful patterns of use or by dependence, as defined by WHO in ICD‑11.

coverage for most antigens (BCG, DTP1, DTP3, HEP3, Hib3, IPV1, IPV2, Polio3, rotavirus last dose, PCV, PCV last dose, and MCV) in 2024, based on official reports from countries. The Region of the Americas leads all WHO regions in postpandemic vaccination recovery.
Immunization coverage data for 2024 indicate a resilient recovery across the Region following the sharp declines observed in 2020–2021 during the COVID-19 pandemic. By 2024, coverage for most antigens had stabilized, reflecting steady progress toward prepandemic levels.
WHO/UNICEF estimates highlighted that the Region of the Americas was the only WHO region where key vaccination indicators surpassed their 2019 levels – a testament to the sustained efforts of Member States and PAHO’s technical cooperation.
The Americas was the first WHO region where key vaccination indicators surpassed prepandemic (2019) levels
Despite overall progress, important gaps remain:
A 5-percentage-point dropout rate between PCV1 and PCV last dose highlights challenges in follow-up, underscoring the need to strengthen continuity of care beyond initial access
At 78%, the vaccination coverage reflects ongoing barriers to timely vaccination of newborns, particularly those born outside health facilities or without early postnatal contact
Remains substantially lower at 79%, leaving critical immunity gaps
Coverage remains below the recommended threshold for population protection, at about 75%
The Region’s strong recovery in vaccination coverage reflects improved access to services, but most antigens have not yet reached 95 %, and subnational coverage remains uneven. Additionally, outbreaks can divert national efforts and resources toward controlling the emergency, pulling attention and workforce away from routine immunization. PAHO continues to work with Member States to close subnational immunity gaps through intensified use of microplanning and promoting geographical information system assisted methods, strengthened surveillance, and ensuring timely outbreak response and preventive vaccination strategies.
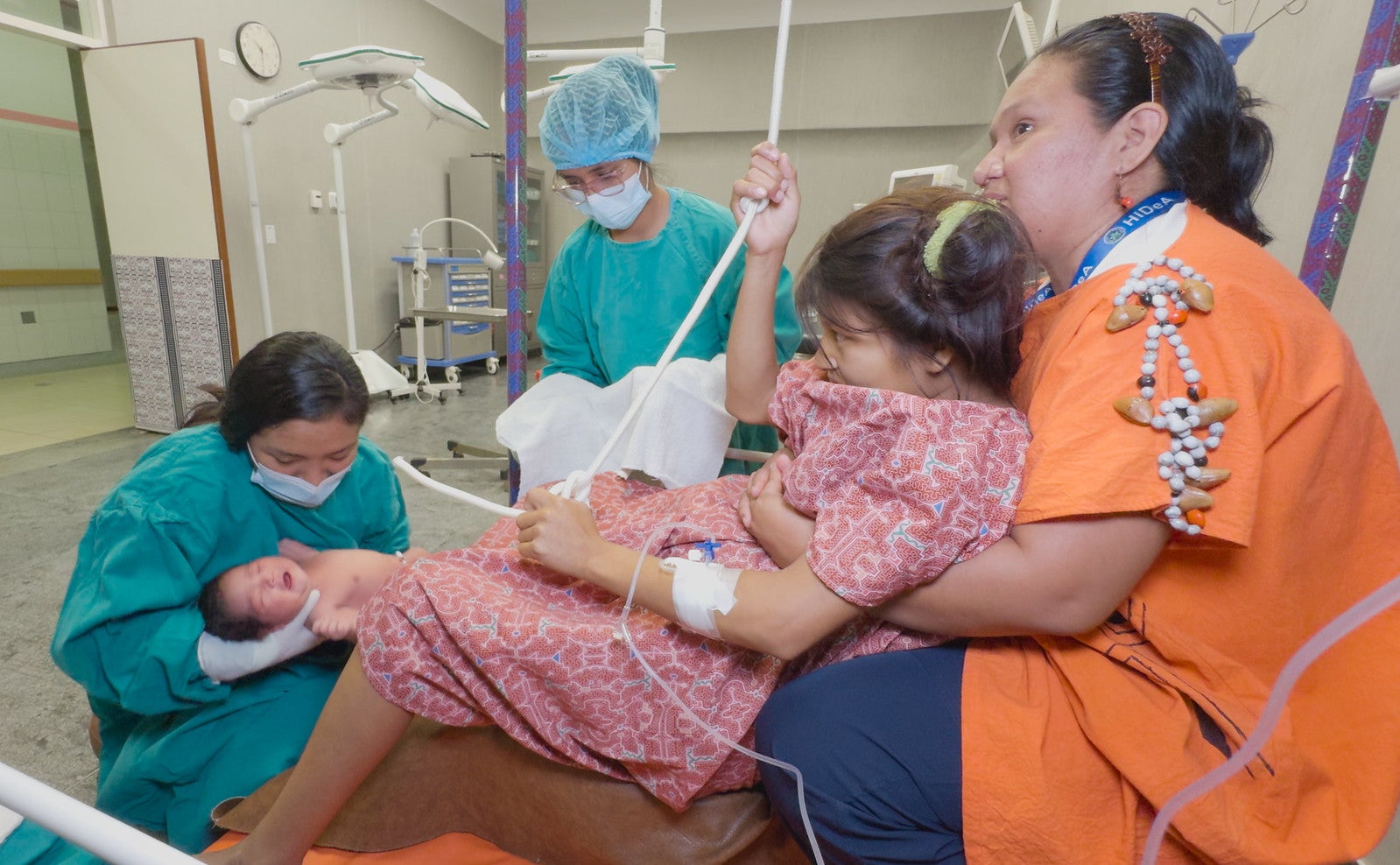
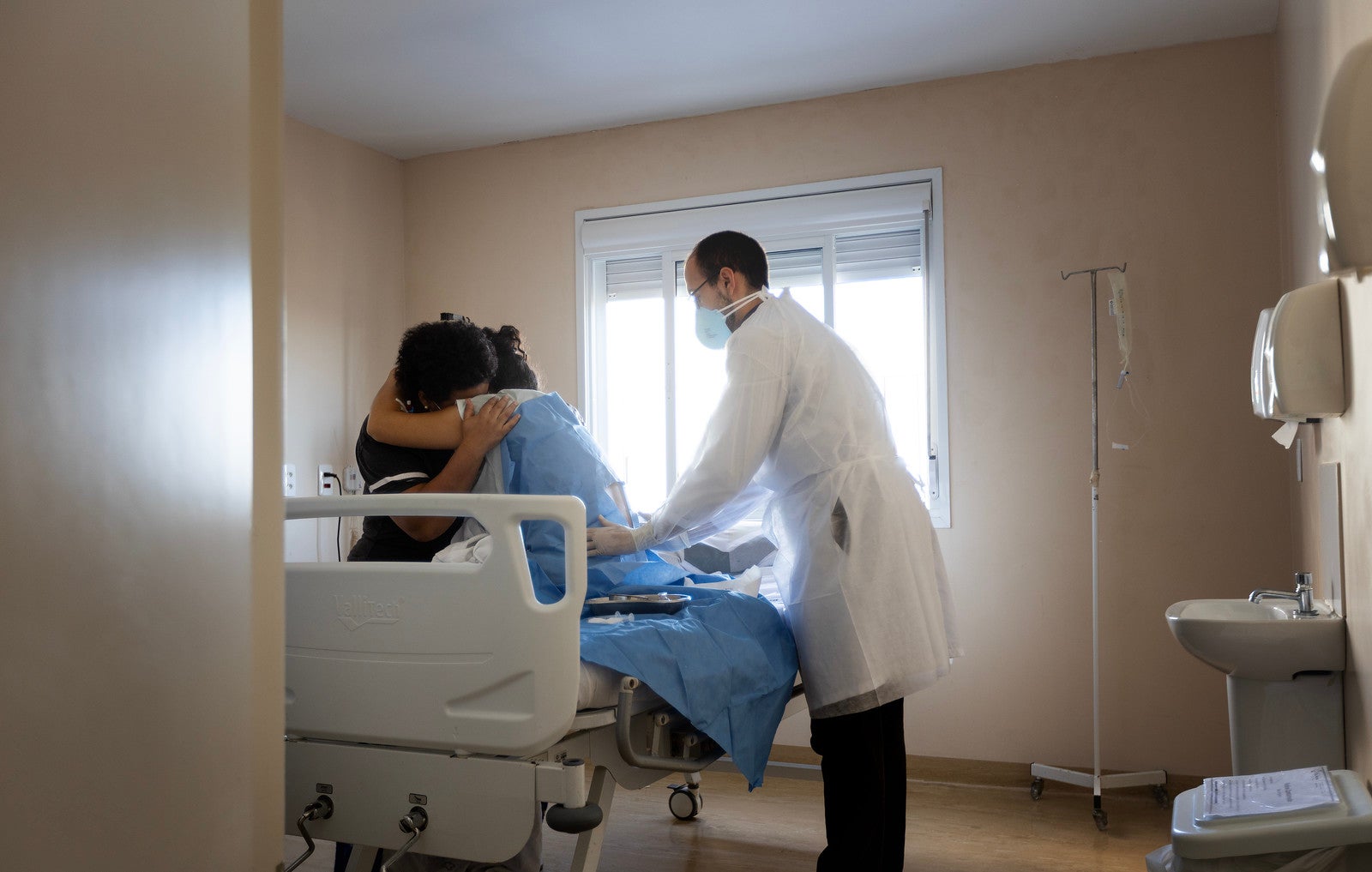
priority countries showed a decrease in the maternal mortality ratio since 2022
In 2024, PAHO’s Director launched the call to action and strategy with 6 strategic lines of action for accelerating maternal mortality reduction, identifying 12 priority countries (Bolivia [Plurinational State of], Brazil, Colombia, Dominican Republic, Guatemala, Haiti, Honduras, Jamaica, Mexico, Paraguay, Peru, and Venezuela [Bolivarian Republic of]) with the highest burden.
Building on the 2024 strategy, PAHO strengthened institutional coordination and accelerated technical cooperation in the 12 priority countries.
Institutional strengthening:
Results in the 12 priority countries:
Despite progress, the Americas recorded only a 16.9% reduction in maternal mortality between 2000 and 2023 – the smallest decline among all WHO regions. In 2023, about 7850 maternal deaths occurred in the Americas, with significant inequalities: a woman’s lifetime risk of dying from maternal causes is 1 in 789 in Latin America and the Caribbean, and 1 in 296 in the Caribbean, compared to 1 in 4322 in North America.

committed by funders’ coalition to implement the Belém Health Action Plan
In 2025, PAHO played a pivotal role in ensuring health was at the forefront of global climate negotiations – culminating in a historic outcome at the 2025 United Nations Climate Change Conference (Conference of the Parties to the UNFCCC [COP30]) in Brazil.
At the request of the Government of Brazil, PAHO provided direct support to the Ministry of Health in shaping the health agenda at COP30, held in Belém, Brazil, in November 2025.
The Belém Health Action Plan provides a concrete road map for countries to build climate-resilient health systems aligned with PAHO’s Policy for Strengthening Equity-Oriented Health Sector Action on Climate Change and Health.
Codeveloping the Belém Health Action Plan and supporting documents
Co-organizing preparatory in-person and virtual events
Preparing for and participating in Health Agenda activities at COP30
Building capacity for early warning and climate-informed health surveillance
Equipping health professionals, and embedding climate into infrastructure and policy frameworks
Mobilizing resilient systems, localized solutions, and health supply chains
New platforms and resources were developed in 2025 to support Member States in achieving their health goals