

PAHO’s flagship initiatives represent its strategic approaches to addressing the Region’s most pressing health challenges. These initiatives reflect how PAHO’s strategy is implemented practically, and range from primarily health initiatives to others that tackle the financial, commercial, and security aspects of health care in the Americas.
Achieving universal health in the Americas is closely linked to transforming health systems through primary health care (PHC). PHC constitutes the backbone of equitable, integrated, and resilient health systems – placing people, families, and communities at the center of care, and serving as both the foundation for and the accelerator of health system transformation.
In the current regional context – marked by demographic transitions, epidemiological and climate-related shifts, postpandemic recovery challenges, and an unprecedented fiscal and economic environment – PHC stands out as the most effective strategy for consolidating health systems capable of responding in an equitable, timely, and sustainable manner.
PHC continues to evolve, increasingly integrating new technologies, digital health tools, and innovative modalities of care to address complex and interrelated challenges while reducing inequities. These changes call for heightened strategic vision, supported by agile governance arrangements and bold public policies.
combined investment portfolio of the Inter-American Development Bank (IDB) and the World Bank in the countries that have joined the Alliance
Countries that are part of the Alliance also worked with resources allocated by the banks in the form of technical cooperation.
The Alliance for Primary Health Care in the Americas was launched in December 2023 by the Inter-American Development Bank (IDB), PAHO, and the World Bank as a unique regional mechanism to accelerate PHC implementation through coordinated policy dialogue, harmonized investment planning, and strategic innovation.
The Alliance is grounded in a shared recognition that resilient, equitable, and people-centered health systems – anchored in the principles of PHC – are essential to achieving universal health and strengthening preparedness for future health emergencies.
Guide and shape investments in health to ensure sustainable financing for PHC services.
Leverage innovative approaches and technologies to enhance the delivery and effectiveness of PHC.
Accelerate health system transformation by implementing policies and initiatives prioritizing PHC.
Three countries have formally joined the Alliance in 2025, establishing permanent national coordination mechanisms (Mesas Consultivas) under the stewardship of their ministries of health:
Chile
Panama
Paraguay
Dominican Republic and El Salvador joined in 2024.
The Alliance is also actively engaged in discussions with 10 additional countries to define pathways for future formal participation: Argentina, the Plurinational State of Bolivia, Brazil, Colombia, Guatemala, Honduras, Jamaica, Mexico, Peru, and Uruguay.
In 2025, the Alliance expanded its engagement in select countries to include ministries of finance through structured discussions with national budget offices, reinforcing the fiscal sustainability of PHC-oriented reforms.
The Lancet Commission report proposes a five-point action plan to guide countries toward people-centered, shock-resilient health systems:
Integrated health service delivery networks represent PHC in action – adapted to the conditions of each territory, translating principles into practice by reorganizing services to guarantee access, continuity, and quality of care for all people.
The updated framework for integrated health service delivery networks highlights:
Integrated health service delivery networks enable priority public health programs to deliver greater impact through integrated service delivery, targeting noncommunicable diseases, communicable diseases, and maternal and child health through an integrated approach.

The Disease Elimination Initiative supports countries and territories of the Americas in eliminating and sustaining the elimination of more than 30 communicable diseases and related conditions by 2030. Launched in 2019, it promotes integrated health services, strong surveillance, and equitable access to prevention, diagnosis, treatment, and care, with a focus on populations in situations of vulnerability.
communicable diseases and related conditions targeted for elimination by 2030
In June 2025, Suriname was certified malaria-free after interrupting local transmission nationwide. This reflects decades of sustained investment in surveillance, timely diagnosis, effective treatment, and outreach to remote populations in Amazonian settings. Twenty countries in the Region have now eliminated malaria.
Brazil received validation in December for eliminating mother-to-child transmission of HIV, meeting required impact and programmatic criteria: incidence rates ≤2%, high coverage of antenatal care, HIV testing, and treatment for pregnant women and infants. Twelve countries have now achieved this milestone, and 11 of those have eliminated mother-to-child transmission of both HIV and syphilis.
In May 2025, both countries were certified free of foot-and-mouth disease in bovids without vaccination, now covering 80% of the Region’s animal population. The Region also celebrated eradication of foot-and-mouth disease virus type C.
Argentina certified the interruption of vector-borne Chagas transmission in 5 new states across 2 provinces and revalidated 2 additional provinces.
In 2025, the Region of the Americas lost its measles elimination status, with Canada becoming an endemic measles country. By year’s end, more than 14 000 confirmed cases had been reported in 13 countries and 30 deaths in three countries, with disproportionate impact on indigenous populations.
This setback highlights the need to sustain high vaccination and homogenous coverage, strong surveillance, and effective rapid outbreak response.
High-level political advocacy, training for ministry of health and health services personnel, systematic epidemiological monitoring, support for vaccination strategies, deployment of consultants for rapid outbreak response, and enhanced communication to reach vaccine-hesitant populations.
Prisons face high burdens of tuberculosis, HIV, sexually transmitted infections, and viral hepatitis due to overcrowding and limited integrated health services. PAHO convened 17 countries for a regional meeting on transmissible diseases in prisons and launched new guidelines. Missions to six countries supported screening, molecular diagnostics, prevention tools (preexposure prophylaxis, postexposure prophylaxis, condoms), hepatitis B vaccination, and expanded hepatitis C treatment.
PAHO supports countries in combining interventions for neglected tropical diseases, malaria, and immunization among indigenous and hard-to-reach populations. This integrated approach addresses high logistic costs, strengthens local capacities, and improves equity in service delivery.
Multiple countries are progressing toward new elimination achievements. Dossiers and national documentation have been submitted or are advancing for:
Several validations and certifications are expected in 2026.

PAHO published one-page, evidence-based briefs summarizing the most cost-effective interventions to accelerate elimination of more than 30 diseases and related conditions – practical guidance for national decision-makers.
Download the PDFFor over 123 years, PAHO and the countries and territories of the Americas have played a key role in realizing historic disease elimination achievements.
Explore Timeline →Digital transformation in health increasingly depends on countries’ ability to move from pilots to sustained implementation at scale. In 2025, PAHO supported Member States with a focus on national and cross-border interoperability, digital documentation of vaccination certificates , highlighting the most recent one for yellow fever, and participation in the Pan-American Highway for Digital Health. These efforts were complemented by actions to strengthen institutional change, workforce readiness, and long-term sustainability.
Priority was given to the practical deployment and adoption of digital solutions as public goods that help to:
Reduce waiting times
Expand access to healthcare specialists
Lower barriers to care, especially in remote and underserved areas
Improve the quality and continuity of health services
Strengthen workforce capacities for the effective adoption of digital health solutions
– while avoiding the widening of existing gaps caused by the digital divide.
Advancing digital transformation in health requires coordinated action across institutions, sectors, and levels of government. Strategic partnerships are a defining element of PAHO’s approach, with the Organization serving as a central convener and trusted platform for aligning technical cooperation, actors, and investments across the Region.
In 2025, PAHO further consolidated its role as a strategic hub for collaboration on digital transformation through a growing network of high-level partnerships aligned around shared regional priorities.
in active technical cooperation financing and loans available through partnerships with Japan, the Republic of Korea, Spain, CAF, IDB, and the World Bank, supporting PAHO-led and co-led initiatives in Member States, including ongoing and new investments in 2025
These coordinated partnerships illustrate PAHO’s unique convening role and capacity to align technical cooperation, technology, and financing within a coherent regional vision.
PAHO’s work in 2025 demonstrates a shift from fragmented digital initiatives toward a robust, interoperable, people-centered, and sustainable digital transformation of public health systems across the Americas.
Priorities for the coming period include:
Continued investment and partnerships will be essential to ensure digital transformation results in more resilient, equitable, and efficient health systems across the Americas. A Regional AI Coalition and Training Program will also be launched in collaboration with key partners across the Americas in 2026.

In the Americas, noncommunicable diseases (NCDs) account for 6 million deaths annually – 65% of all mortality in 2021, and eventually expected to exceed 80% of all deaths – with 38% occurring prematurely in people under 70. About 240 million people live with at least one NCD, making these conditions the leading cause of death and disability in the Region.
The Better Care for NCDs Initiative aims to strengthen the capacity of health authorities to integrate comprehensive NCD services into primary health care (PHC), improve screening, diagnosis, treatment, and follow-up, and strengthen data collection and monitoring of outcomes.
The targeted areas are:
For governments
Strengthen national capacity to plan and integrate comprehensive NCD services into PHC.
For PHC services
Increase capability to deliver quality NCD screening, diagnosis, treatment, and continuous follow-up care, including referral systems.
For healthcare facilities
Strengthen data collection and monitoring of NCD diagnosis, treatment, and care outcomes.
Through the Regional Revolving Funds, 32 countries are procuring NCD-related medicines and technologies for PHC. Specifically for hypertension, diabetes, and cervical cancer:
About 50 000 healthcare providers completed the introductory course on Better Care for NCDs. A learning pathway of 20+ courses has been developed through the PAHO Virtual Campus, with over 500 000 health professionals completing courses across NCD topics.
Despite significant progress, several ongoing challenges require attention:
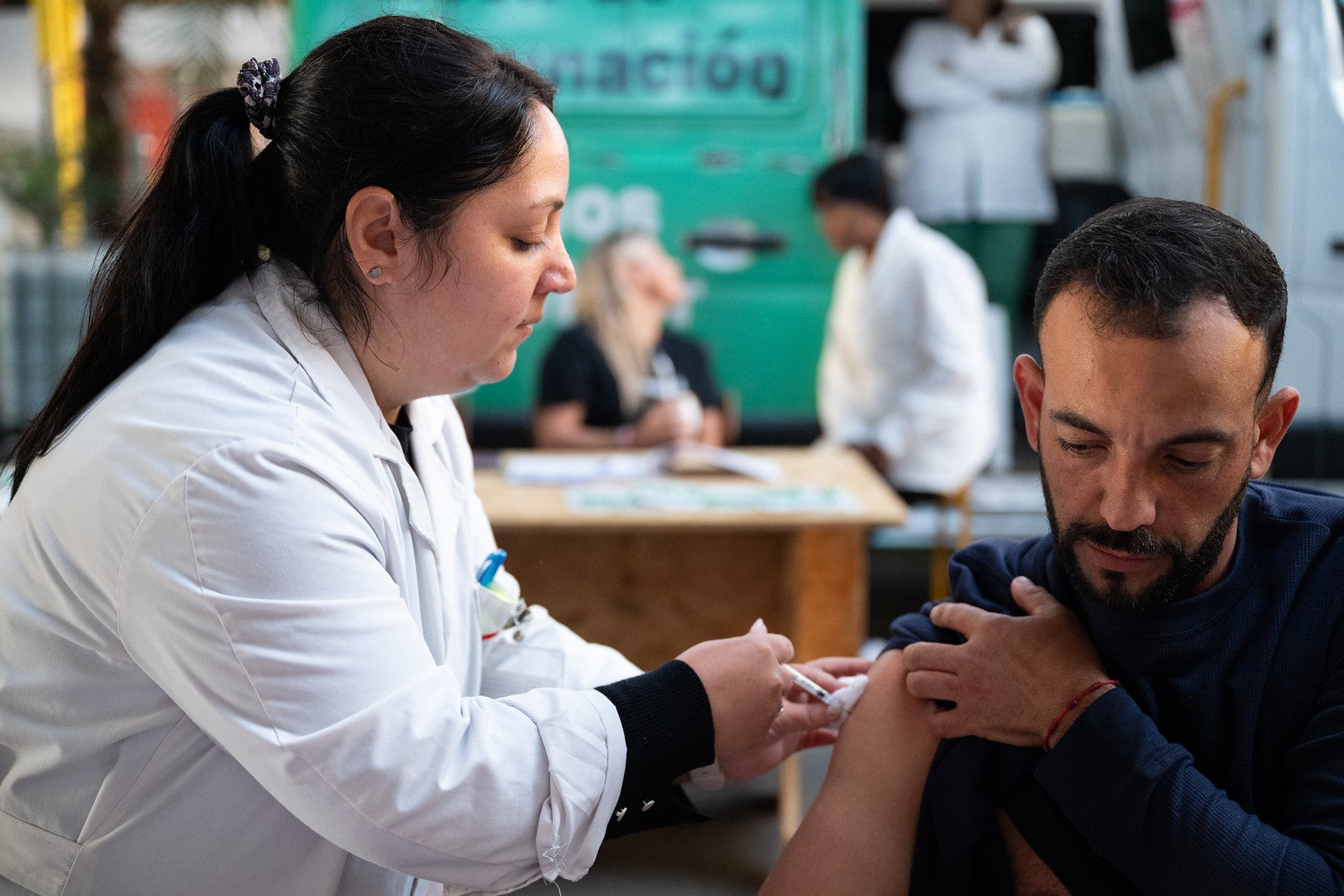
In 2025, the Regional Revolving Funds (RRFs) continued their role as the Region’s most powerful mechanism for collective procurement – ensuring that all countries, regardless of size or resources, can access quality vaccines, medicines, and medical equipment at affordable prices.
With more than 60 years of combined experience, the RRFs are technical cooperation mechanisms comprised of:
Access to vaccines, cold boxes, and syringes.
Access to essential medicines, diagnostics, and medical equipment.
The RRFs play a critical role in supporting regional production by consolidating demand and providing market predictability for local manufacturers. In 2025, regional manufacturing projects advanced to include additional locally produced vaccines, building on the successful Pfizer-Sinergium-Argentina collaboration for PCV20 signed in January.
In 2020, regional vaccine producers supplied just 1.5% of the volume and 0.3% of the value of vaccines procured through PAHO’s Regional Revolving Funds.
By 2025, regional manufacturers were able to supply 26% of the volume and 30% of the value of regional demand.

Latin America and the Caribbean have existing capacities in health technology innovation and production. However, access to regionally produced health technologies remains limited, reflecting structural constraints in regional value chains, trade integration, and productive scale. The region continues to face significant dependence on external sources for vaccines, medicines, active pharmaceutical ingredients, and other critical inputs.
The COVID-19 pandemic underscored the risks of this dependence. Beyond the pandemic, emerging health threats and geopolitical pressures on global supply chains further highlight the need to strengthen regional production as a core component of health security.
Through sustained political commitment, strengthened governance, and coordinated regional action, Latin America and the Caribbean are building the foundations for greater self-sufficiency in health technologies.
In 2025, the Regional Revolving Funds (RRFs) procured about 25% of the demand for influenza vaccines from regional manufacturers. During that same year, the RRFs entered agreements with regional manufacturers to supply up to 65% of the demand effective from 2026 onward.
This represents a fundamental shift to a significant regional supply capacity.
Producers in 7 countries operate more than 30 public and private facilities across different segments of the vaccine production value chain.
Four public and private producers have advanced in constructing new infrastructure to produce vaccines based on mRNA platforms.
Regional manufacturers have initiated more than 30 research, development, and production projects for vaccines and other mRNA health technologies.
Production of active pharmaceutical ingredients remains a regional challenge, with external dependence estimated at 85% in Argentina and 95% in Brazil.
While aggregate export volumes remain low, 54% are destined for markets within the Latin America and Caribbean region– demonstrating the potential of the regional market as a platform for growth.
In 2021, the PAHO Directing Council approved the resolution Increasing Production Capacity for Essential Medicines and Health Technologies (CD59.R3). In 2023, PAHO launched the Innovation and Regional Production Platform. In 2024, Member States adopted resolution CD61.R14, establishing flexibilities for PAHO’s Regional Revolving Funds to encourage regional production.
PAHO continued expanding strategic partnerships with Canada, the European Union, Mercosur, the Spanish Agency for International Development Cooperation, Africa Centres for Disease Control and Prevention, the Coalition for Epidemic Preparedness Innovations, the Latin American Association of Pharmaceutical Industries, the Latin American Federation of the Pharmaceutical Industry, and the Regionalized Vaccine Manufacturing Collaborative, reinforcing collaboration to advance regional innovation and production.