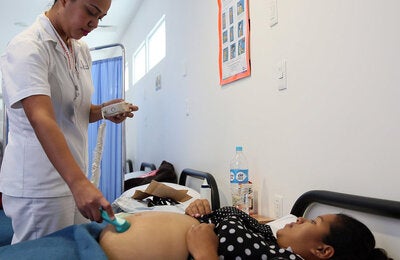
Georgetown, 6 November 2020 (PAHO/WHO)—In 2018 the Director of PAHO, Dr. Carissa Etienne identified Guyana as one of the 10 countries in the Caribbean and Latin America with the highest Maternal Mortality Ratio that needed urgent attention. As a result of this, a special department was created in Guyana’s PAHO country office to specifically address all matters directly related to Maternal Mortality.
Over the last 2 years PAHO has worked closely with the Ministry of Public Health in implementing various evidence based strategies to work towards quickly reducing Maternal Mortality in Guyana. The Zero Maternal Death from Hemorrhage strategy was implemented across all 10 regions of the country and 100 non pneumatic anti shock garments were donated. Following this there was a drastic reduction of maternal deaths from post-delivery bleeding, which accounted to a vast number of women dying in Guyana in 2018.
The country now has certified medical workers for the insertion and removal of modern long acting reversible contraception thanks to training provided by the Latin American Center for Perinatology CLAP/PAHO. These are only a few examples of capacity building that was done to help improve patient care and ensure safe deliveries of our mothers.
The COVID-19 Pandemic brought with it many challenges to ensuring continuity of optimal care at all levels but especially as it concerns pregnant mothers. PAHO continued to work closely with the Maternal Child Health Department at the MoPH to develop operation guidance for MCH services during COVID-19. Additionally, active surveillance and follow up of COVID-19 positive pregnant patients is done. To date, Guyana has 206 confirmed cases of COVID-19 of which 2 were pregnant mothers both are now recovered from the infection and one has successfully delivered.
Signs and Symptoms and a Novel Disease
Krystle Halley-Ifill a 27-year-old nurse was the first pregnant patient diagnosed with COVID – 19 in Guyana. Her source of contact was her husband with whom she, her mother-in-law and her 1-year-old son shared a home. Her Husband, Jermaine Ifill, was an emergency Medical Technician by profession and in March started with flu like symptoms. At first, Krystle and Jermaine though that it was pneumonia, since he would often have similar episodes and was having difficulty breathing.
Krystle accompanied her husband to the emergency room where he was admitted due to the difficulty breathing and was given oxygen and taken to the male ward. Two days after he was admitted, he was given a COVID-19 test of which returned positive. After her husband was diagnosed with COVID-19, the hospital made contact with her and her family whom she lived with at the time and both herself and her mother-in-law were tested and found to have COVID-19. The two children who lived with them at the time both tested negative for COVID - 19. Unfortunately, four days after Krystle’s husband received his results, he died.
Treatment at the Diamond Isolation Centre
The news of her husband’s death made it more difficult for Krystle to cope, since she was not with her husband when he died. Krystle was in her third trimester of her pregnancy when she was diagnosed positive for COVID-19 on 30 March, even though she was asymptomatic. Krystle was admitted to Diamond Diagnostic Centre for isolation, where she received ongoing antenatal care. The fear of her baby contracting the virus was a deep concern for Krystle however, she spent 30 days in isolation and care until she was tested negative and cleared of the infection.
In sharing her story, she mentioned that she received lots of support from her family and the staff at the Diamond Diagnostic Centre, where she was isolated. On the 30 April, Krystle was discharged from the Isolation facility and continued her pregnancy healthy and COVID-19 free.
Stigma and Discrimination
One of the main issues for those suffering with COVID-19 is the challenge they face going about their daily lives, especially when persons around them are aware of them having the virus.
According to Krystle living a normal life after testing positive for COVID-19 was far from normal, hence, from her recollection, friends and family turning their back on she and her family brought much sadness to her, “when my husband was diagnosed with COVID-19 there was immediate distancing from people who we know. My family who lives in Berbice also faced discrimination through the people who we were close and some of my friends who found out that I had COVID-19. They did not want to go near my family, even though I was living in Georgetown, which was miles away from Berbice, at the time when I had COVID-19”. However, the fear of discrimination is certainly not un-common among the patients at the Isolation sites, who often find the stigma overwhelming.
Life after COVID-19
On 19 May, Krystle delivered a bouncing, healthy baby boy. Both baby and mom are doing well. Krystle and her sons are now with her family in Berbice, continuing with their lives, through this difficult time of her not having her husband and the father of her children around to lean on and to enjoy the new addition to the family.