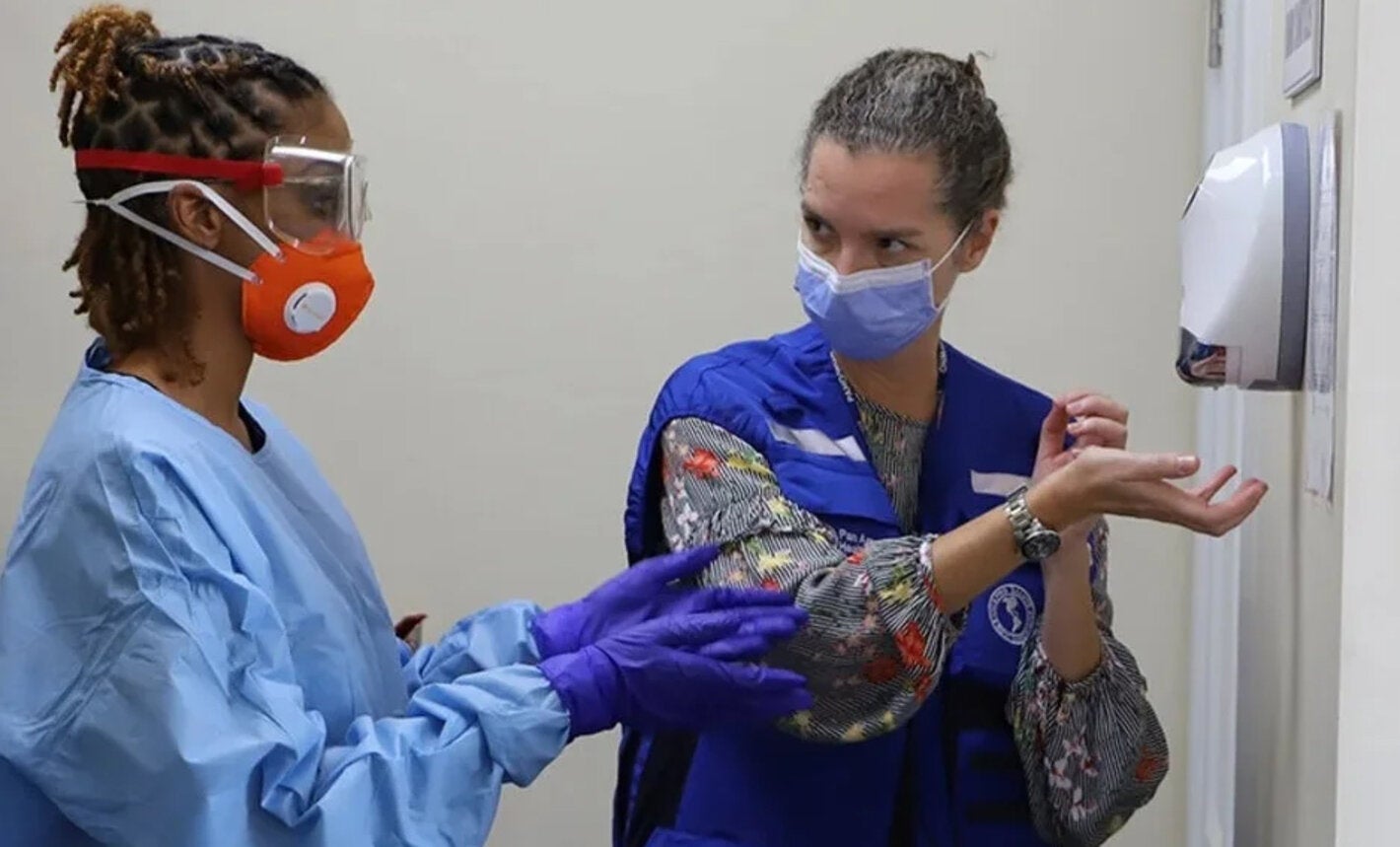
Infection prevention and control (IPC) is an evidence-based approach that prevents patients and health workers from being harmed by avoidable infection and as a result of antimicrobial resistance. IPC is essential to the work of the PAHO/WHO Country Office serving Jamaica, Bermuda and the Cayman Islands.
This week, we had a quickfire interview with Dr. Stempliuk, the Advisor for Health Surveillance, Disease Prevention and Control at the Country Office and Infection Prevention and Control Team Lead for PAHO’s regional COVID-19 Incident Management Support Team. Dr. Stempliuk has worked in infection control for over twenty years, first in Brazil, several countries in the Caribbean and Latin America, and at the Pan American Health Organization (PAHO) Headquarters.
Q: What are healthcare-associated infections (HAI)?
A: HAI are infections that patients acquire after being admitted to the hospital as a consequence of hospitalization or a medical procedure. Up to 50% of those infections are preventable by implementing evidence-based measures. These measures include proper hand hygiene and isolation of patients with communicable diseases, and other specific interventions for preventing the acquisition of pneumonia, urinary tract infection or bloodstream infection.
Q: Why is HAI important in the context of COVID-19?
A: The COVID-19 pandemic response has put health systems under extreme pressure. There are many risk factors to acquire HAI, among them we noted that two increased during the pandemic.
One is understaffing of healthcare facilities. As many health care workers become ill from COVID-19, it left health centers with reduced numbers of staff.
The second risk factor is the severity of patients. We noted an increase during the pandemic as hospitals received more patients experiencing severe COVID-19 presentations and who required admission into the intensive care unit (ICU).
Under these conditions, we must double our efforts to prevent HAI during this challenging time.
Q: What are three recommendations for the prevention of healthcare-associated infection (HAI) in admitted patients in acute care facilities?
A: HAI represents a large group of infections that we put under the same title. All recommendations must be tailored at the local level to support implementation by health services and at the clinical level.
The first recommendation is to have a trained infection prevention and control team in hospitals at the health services level. This team will make recommendations at the local level, train health care workers, follow up, and monitor the results of the measures implemented.
The second will be an implementation of standard precautions. These precautions are a group of practices to avoid transmission of infections in health care facilities which includes implementation of transmission-based precautions, or isolation, to avoid cross-infection in health care facilities and outbreaks.
For health care workers, the recommendations are to perform hand hygiene following the World Health Organization’s five moments for hand hygiene; correct use of personal protective equipment (PPE); and perform critical procedures maintaining the asepsis required.
Q: At the recent, HSS Pillar Training titled, Prevention of Healthcare-Associated infection in an admitted patient with COVID19, you delivered a presentation on the prevention of respiratory tract infections, what key takeaways did you want people to gain from your presentation?
A: The HSS Pillar Training was part of a three-day webinar series discussing the prevention of HAI in the ICU. On the first day, we discussed the prevention of bloodstream infections, on the second day we discussed the prevention of respiratory tract infections, and on the final day, we focused on the prevention of urinary tract infections. All speakers reinforced the existing recommendations for the prevention of bloodstream, respiratory and urinary tract infections.
In the case of respiratory infections, we must work to guarantee prevention of aspiration, minimize ventilation days, reduce the pathogen load, practice safe endotracheal suction practices, and apply pharmaceutical preventive measures. The COVID-19 pandemic has changed the working environment for health care workers, with much more patients to care for and their own increased vulnerabilities. Therefore, education and monitoring need to be reinforced to guarantee that health care workers are performing their best to prevent respiratory infection and other HAI.



