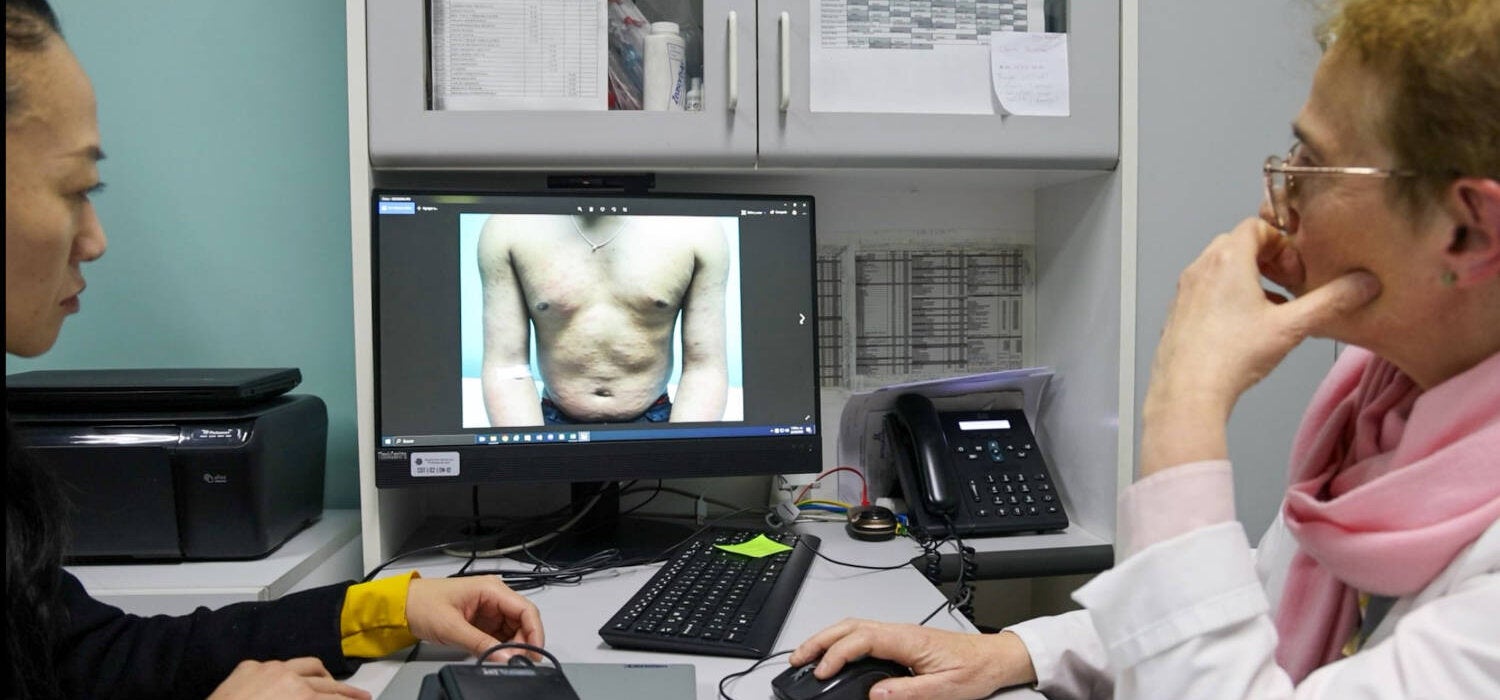
With strong surveillance, political commitment, and support from PAHO, Chile has become the first country in the Americas to achieve elimination status.
— March 2026 —
In Chile’s health system, leprosy has been out of sight, but it has not been out of mind.
There have been no autochthonous cases for over 30 years, and unlike many diseases that fade from view as cases decline, leprosy was never allowed to disappear from Chile’s health system. It remained notifiable, meaning health professionals and laboratories are legally required to report confirmed and suspected cases to public health authorities. Due to this, it remained monitored and a part of institutional memory—even as most clinicians would never encounter a case in their careers.
“A major challenge, when you reach this level of elimination, is maintaining awareness of neglected diseases like leprosy,” explains Patricia Contreras, Head of Chile’s Department of Communicable Diseases at the Ministry of Health. “Even if we see very few cases—or none at all—we must be prepared to recognize, remember, and identify a case, and have the capacity needed to respond and provide holistic care.”
Leprosy, also known as Hansen’s disease, is one of the world’s oldest neglected tropical diseases (NTDs)—a group of preventable and treatable conditions that continue to affect millions of people, particularly those living in poverty and with limited access to health services.
Globally, there are leprosy cases in more than 120 countries, and around 200,000 new cases reported every year. The region of the Americas accounts for approximately 13% of all reported cases worldwide. The elimination of leprosy is defined as: zero new autochthonous cases for at least three consecutive years after having interrupted transmission for at least five years.
Every case of leprosy in Chile triggers surveillance, investigation, treatment, and follow-up, reinforcing a system designed not for volume, but for vigilance. Surveillance data show that between 2012 and 2023, a total of 47 cases were reported nationwide, all of them imported. Most occurred in men and were concentrated in the Metropolitan Region of Santiago.