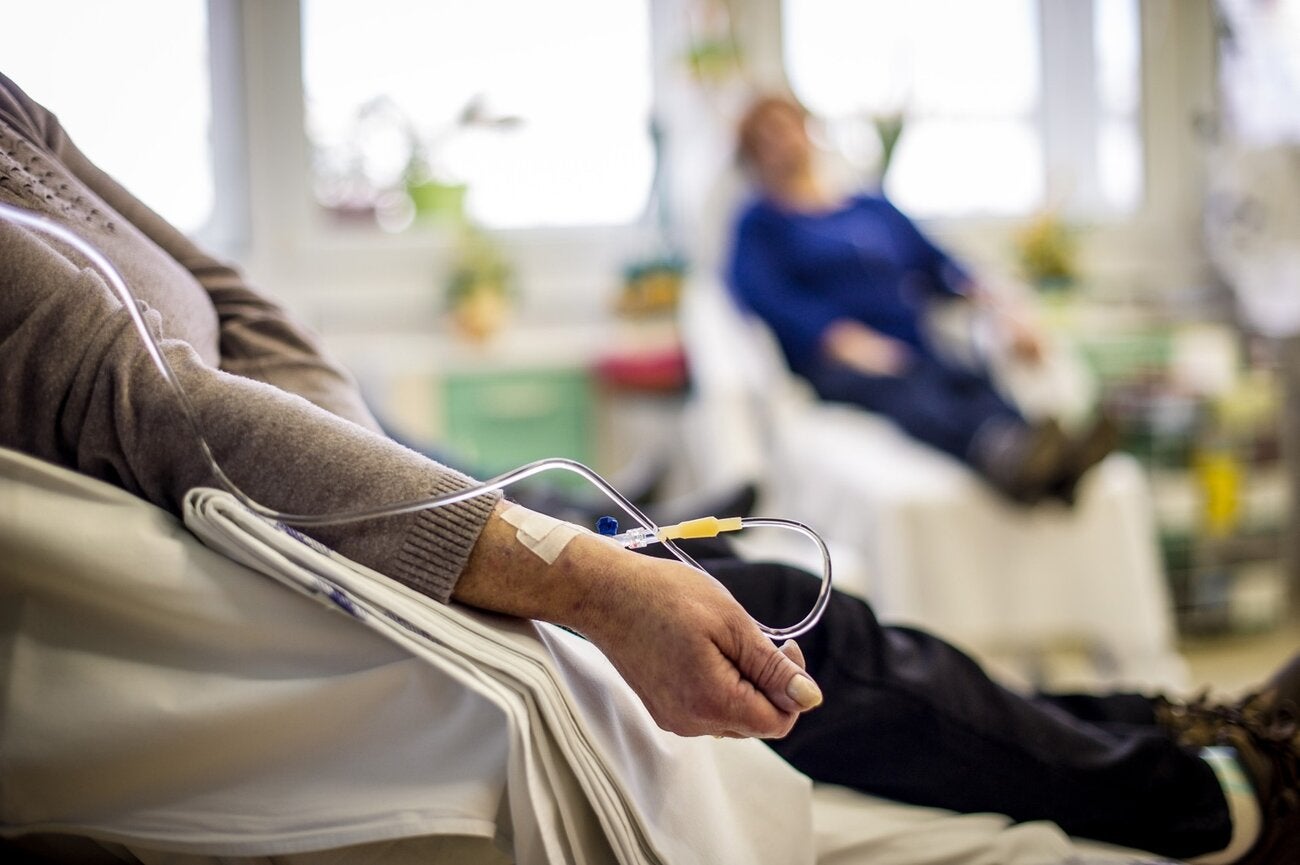
Cancer in the Americas
In the Americas, cancer is the second leading cause of death, where are an estimated 4 million people were newly diagnosed and 1.4 million people died from the disease in 2020. Approximately, 57% of new cancer cases and 47% of cancer deaths occurred in people 69 years of age and younger, in the prime of their lives.
The most frequently diagnosed types of cancer among men are: prostate (21.7%), lung (8.9%), colorectal (7.8%), bladder (4.5%) and melanoma of the skin (3.4%). Among women, the types of cancer with the highest incidence are: breast (25.4%), lung (8.5%), colorectal (7.9%), thyroid (5 %) and cervical (3.8%)
The type of cancers with the highest mortality in men are: lung (18%), prostate (11.1%), colorectal (9.4%), liver (6.1%) and stomach ( 5.6%). The cancers that cause the most deaths among women are: breast (13.2%), lung (12.3%), colorectal (7%), cervicouterino (5.3% ) and ovary (3,9%)
Future trends
Globally, there were an estimated 20 million new cases of cancer and 10 million deaths from cancer. the cancer burden will increase by approximately 60% over the next two decades, further straining health systems, people and communities. The predicted global burden will increase to about 30 million new cancer cases by 2040, with the greatest increases occuring in low- and middle-income countries.
In the Americas region the, number of people expected to be diagnosed with cancer will increase by 55%, to approximately 6.23 million people are predicted to be diagnosed with cancer by 2040, if no further action is taken to prevent and control cancer.
C
Cancer can be prevented and controlled
Cancer can be prevented and controlled by implementing evidence-based strategies for cancer prevention, screening and early detection, treatment and palliative care. The most common modifiable risk factors for cancer, which are shared with many other noncommunicable diseases, are:
- Tobacco use
- Low fruit and vegetable intake
- Harmful use of alcohol
- Lack of physical activity
Some specific risk factors for cancer include chronic infections from human papilloma virus (HPV) -for cervical cancer-, hepatitis B and C - for liver cancer-, and H.pylori -for stomach cancer.
One third to one half of cancer cases could be prevented by reducing the prevalence of known risk factors. Examples of actionable interventions are tobacco control and HPV vaccination. The most effective primary prevention of cancer is based on whole-of-government approaches, with legislation, regulation and fiscal policies combined with activities to change community and individual behaviour. Public health messages and health promotion should present evidence on specific risk factors.
PAHO/WHO is working with its member countries in different aspects related to cancer prevention and control.
Cancer can be prevented and controlled by implementing evidence-based strategies for cancer prevention, screening and early detection, treatment and palliative care.
Scaling-up cancer control to achieve universal health coverage (UHC) is essential to improve health outcomes and save lives in all countries. Cancer services should be included in UHC benefits packages to ensure access to essential treatment and care.
Developing a national cancer control plan is beneficial to identify the priority policies, services and actions for cancer prevention, screening, early detection, diagnosis, treatment and palliative care.
Late- stage diagnosis is common, especially where health systems are not robust. Effective early cancer diagnosis can be achieved through raising public and health professional awareness of cancer signs and symptoms, establishing referral systems, offering rapid clinical and pathological diagnosis, and appropriate treatment and supportive care.
Several cancer types, notably cervical, breast and colorectal cancers, can be detected in early stages through screening asymptomatic people with cost-effective screening tests; and coupled with diagnosis and treatment, can save lives.
Programs need to improve quality of cancer care. Quality can be improved by regulatory interventions, national policies, clinical practice guidelines and enhanced training of the healthcare workforce.
The vast majority of cancer patients lack access to palliative care, resulting in painful deaths. Palliative care should be a health care priority.
PAHO works to build capacity on palliative care, developing virtual courses and collaborating with other partners in facilitating online learning networks. Learn more at Palliative Care
Planning cancer control starts with the collection and analysis of data on trends in incidence and mortality, the prevalence of risk factors and current capacity and system performance. In this regard, cancer registries are an important part of cancer control.
CANCER AND COVID-19
People with cancer are at increased risk of severe COVID-19, and people who have COVID-19 and an underlying condition such as cancer have higher mortality than those without cancer. COVID-19 has disrupted essential health services, including cancer care.
Delays in cancer diagnosis and treatment have an impact on the progression of cancer, and during the COVID-19 pandemic delays in cancer care could lead to future peaks in mortality from potentially curable cancers, as a result of not receiving standard treatment. For this reason, cancer services should rapidly manage and avoid any cumulative delays in treatment and prevent an increase in avoidable deaths from cancer. Preventing COVID-19 infection in centers where cancer services are delivered is crucial for protecting patients and health center workers. Efforts should be made to maintain treatment objectives and control symptoms and complications.
Given the vulnerability of cancer patients, it is recommended that services continue the reorganization process until there is reduced risk of COVID-19 infection during the pandemic.
RESOURCES
A global strategy for the elimination of cervical cancer
Approximately 72,000 women were diagnosed with cervical cancer in 2018 and almost 34,000 died from it in the Region of the Americas. Cervical cancer is preventable through HPV vaccination and also with screening and treatment of precancerous lesions, It can be effectively treated if diagnosed in its early stages.
In August 2020, the World Health Assembly passed a resolution calling for elimination of cervical cancer and adopting a strategy to make it happen.The Global Strategy has three main pillars: prevent, screen and treat, that capture a comprehensive approach that includes prevention, effective screening and treatment of pre-cancerous lesions, early cancer diagnosis and programmes for the management of invasive cancer.
PAHO joins the efforts to implement the Global strategy in the Region of the Americas and has also developed a communications campaign with materials, information and stories available for Ministries of Health and health institutions to promote cervical cancer prevention through HPV vaccination and screening and treatment of precancerous lesions.
Now is the time to end cervical cancer