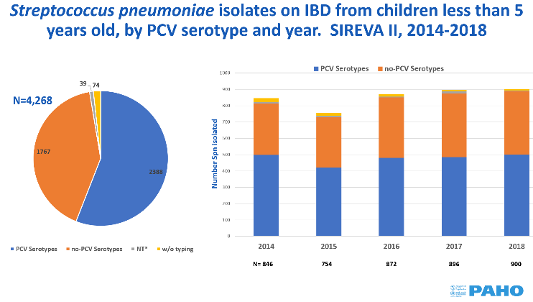
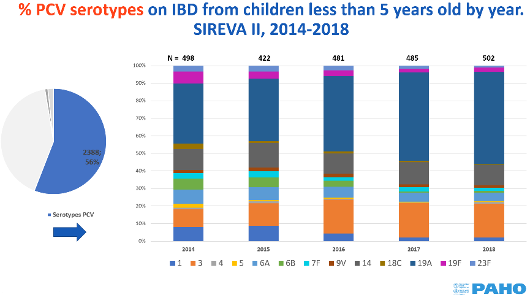
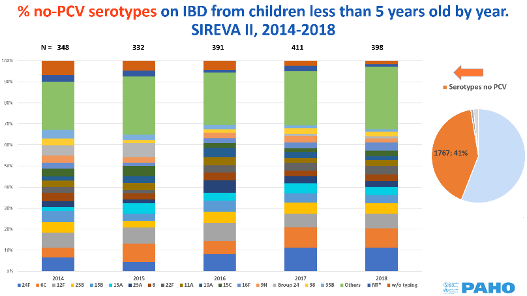
Pneumococcus is a Gram-positive lancet-shaped diplococcus with a polysaccharide capsule external to the wall. According to the capsular antigenic differences, more than 90 serotypes have been identified, of which a limited number cause invasive pneumococcal disease. Serotype identification has varied by geographic region, age, and study period; 6 to 11 of the most common serotypes cause approximately 70% of all invasive infections in children worldwide.
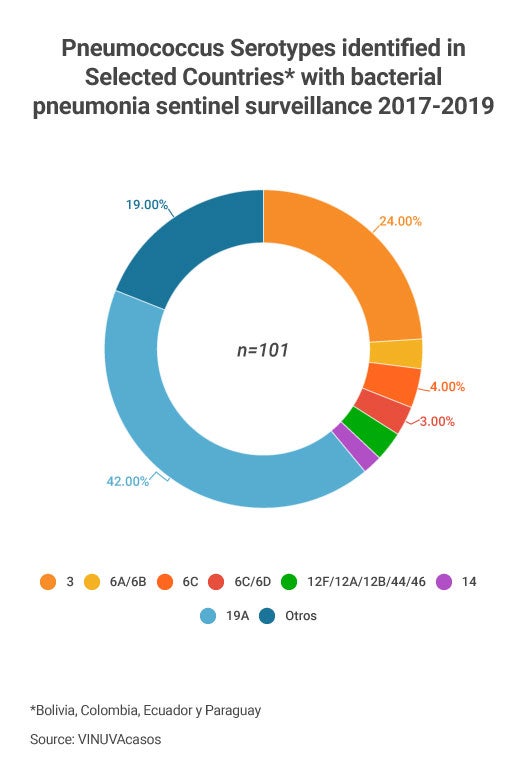
- Pneumococcal is the second agent causing community-acquired pneumonia (CAPs) and requiring hospitalization after the Respiratory Syncytial Virus (RSV).
- More than 95% of all episodes of clinical pneumonia and more than 99% of pneumonia deaths among children under 5 acute occur in developing countries. At the same time respiratory infections, especially CAPs, are the leading causes of hospitalization and death among children under five years of age in these countries.
- In the Region of the Americas, the pneumococcal infection incidence rate in 2015 was estimated to be 358 cases per 100,000 children under 5 years of age and have caused around 5,700 deaths occurred
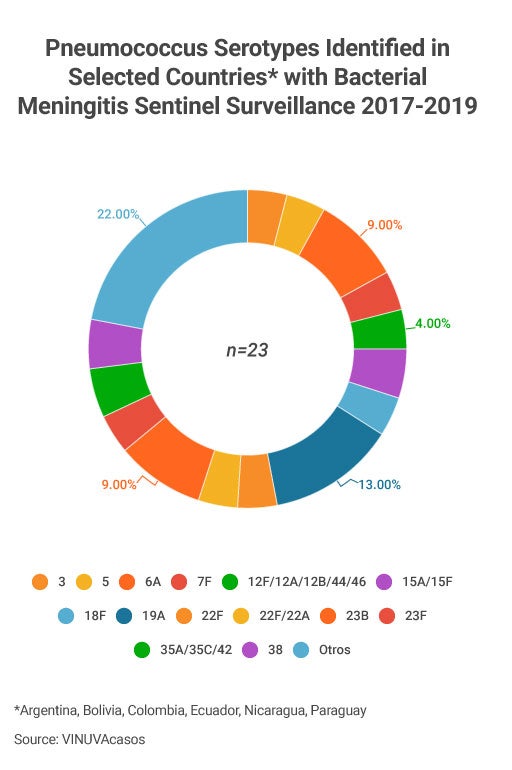
- Among the causes of death due to pneumococcal infection, pneumonia represents 81% and meningitis 12%. As for bacterial meningitis in children under 5, there are approximately 1.2 million cases and 180,000 deaths annually.
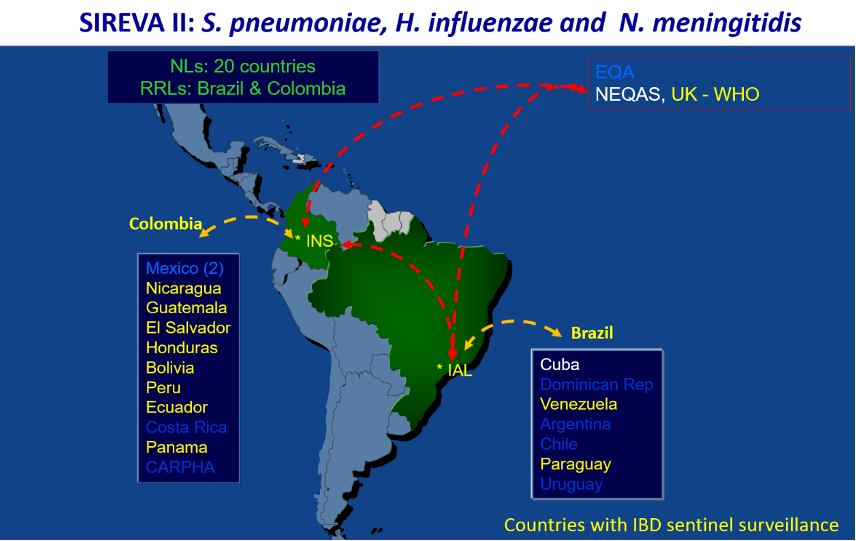
- In an analysis published in 2013, the Region of the Americas had the lowest burden of disease worldwide, with an incidence of 17 cases per 100,000 children per year. It is estimated that, globally, more than 90% of bacterial meningitis is caused by S. pneumoniae, H. influenzae and N. meningitidis. Currently, in the Region of the Americas, S. pneumoniae is primarily responsible for bacterial meningitis.
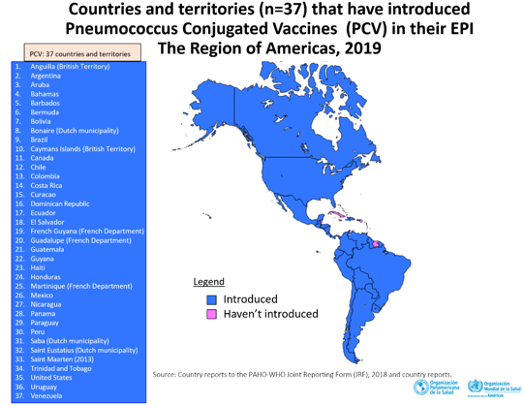
- The pneumococcal conjugate vaccine (PCV) was introduced in the Region in the year 2000, as of December 2019, 37 countries and territories in the Region have introduced one of the two pneumococcal vaccines in their regular programs.
Susceptibility to pneumococcal infections is universal; that is everyone is generally susceptible to infections caused by this agent. However, some conditions increase susceptibility to this bacterium, including invasive diseases: age, chronic disease, overcrowding, poverty, active or passive exposure to tobacco smoke, and concurrent upper-respiratory-tract infections. Pneumococcal infection is more frequent between the ages of 2 months and 3 years, although its incidence decreases after 18 months of age. The risk increases again after the age of 65.
Pneumococcal disease is transmitted directly (person to person) or through contact with nasopharyngeal secretions(droplets) from the person infected.
Pneumococcal disease is distributed worldwide and is present in every climate and season. In countries with a temperate climate, an increase in the incidence of pneumococcal pneumonia is seen in winter and spring.
Immunity to pneumococcus can be acquired passively through the placenta, or actively by previous infection or immunization. Newborns can have antibodies due to passive transmission from the mother. However, they disappear within months, as the incidence of the invasive disease increases.
After the age of 18 months, children show specific immune responses to the majority of the circulating pneumococcus serotypes, as a result of repeated exposure.