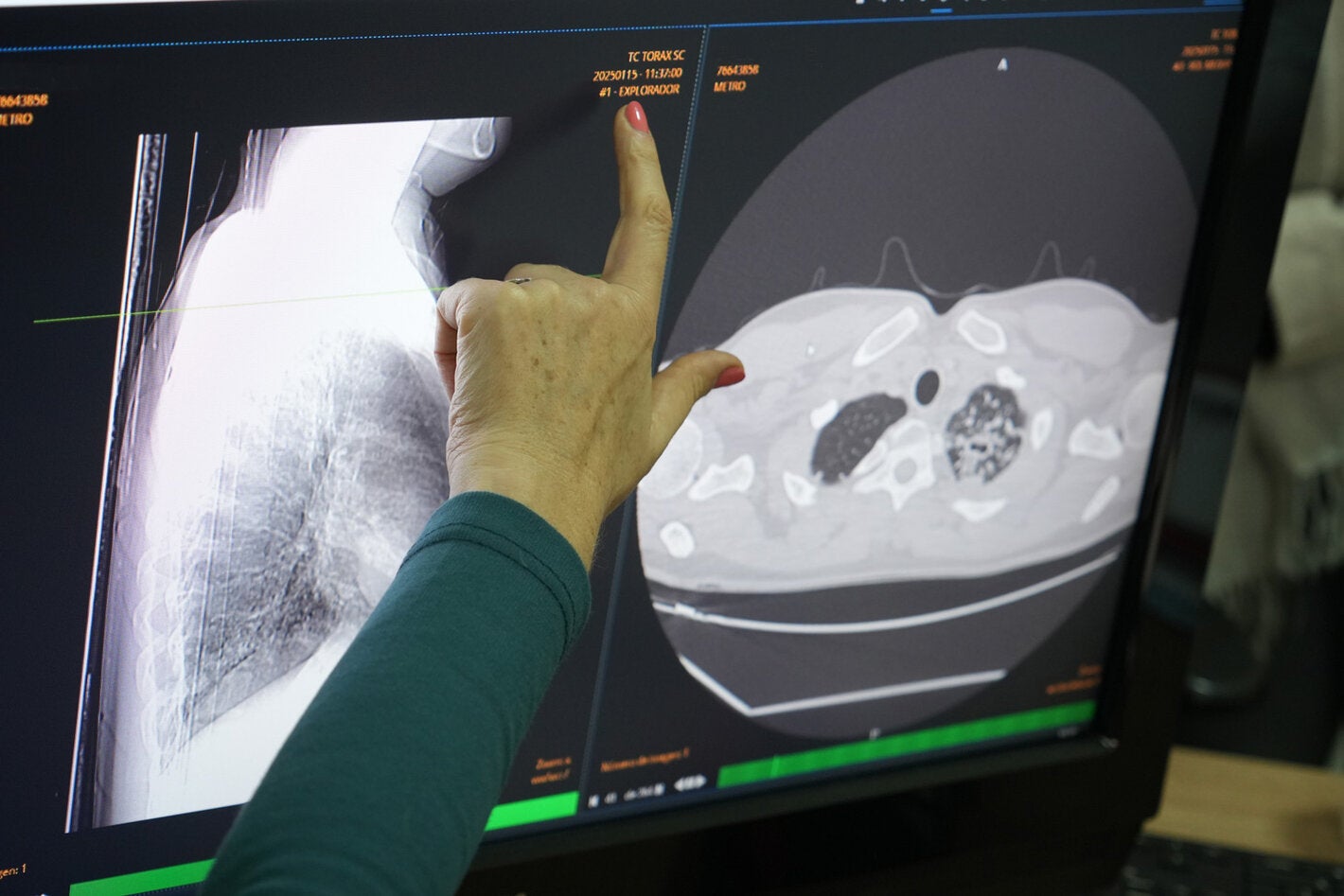
In the Americas, an estimated 350,000 people fell ill with tuberculosis in 2024, and nearly 77,000 were not diagnosed, highlighting the need to bring diagnosis and treatment closer to communities.
Washington, D.C., March 24, 2026 (PAHO) – Each year on March 24, World Tuberculosis Day is observed as an opportunity to raise awareness about a preventable and curable disease that continues to pose a significant public health challenge in the Americas.
In this context, Dr. Pedro Avedillo, Regional Advisor for Tuberculosis Prevention, Control, and Elimination at PAHO, shares insights on the current situation of the disease, recent advances, and the role of primary health care in bringing diagnosis and treatment closer to people, reducing gaps, and advancing toward elimination.
What is the current situation of tuberculosis in the Americas?
In the Region of the Americas, an estimated 350,000 people fell ill with tuberculosis and around 30,000 died from the disease in 2024. Of these deaths, approximately 29% were attributed to TB-HIV coinfection.
That same year, an estimated 77,000 people with tuberculosis (about 1 in 4) were not diagnosed, meaning many continued without treatment and may have kept transmitting the disease.
Despite being preventable and treatable, why does tuberculosis remain a public health problem?
In recent years, we have seen some stabilization in TB incidence and mortality, along with an increase in the number of diagnoses and people receiving treatment. This reflects efforts to strengthen the response, for example by expanding rapid molecular testing for diagnosis and introducing shorter treatment and prevention regimens.
Tuberculosis remains closely linked to poverty, overcrowding, malnutrition, and barriers to accessing health services. Many people with symptoms are not diagnosed in time or interrupt treatment, allowing transmission to continue in the community.
Other factors also play a role, such as HIV coinfection, drug-resistant TB, and disruptions in health services like the ones seen during the COVID-19 pandemic.
One of the main challenges is timely detection. Why is early diagnosis so important?
Diagnosing tuberculosis early reduces transmission of the bacteria to others and allows treatment to begin before the disease causes more serious complications. When diagnosis is delayed, the infection can progress and spread to other organs, increasing the risk of long-term sequelae. Early detection remains one of the most effective strategies for working towards elimination of the disease.
What recent advances have been made in TB prevention and treatment?
In recent years, several important innovations have emerged. One is the use of digital radiology with AI-assisted reading, which enables more timely screening and brings diagnosis closer to those who need it most. Rapid molecular tests have also expanded; they are highly sensitive and can be used near the point of care, significantly reducing the time needed to confirm diagnosis.
In terms of treatment, fully oral and shorter therapeutic regimens are now available, both for treating the disease and for prevention in people at risk. These options make it easier for patients to adhere to treatment and improve outcomes.
What role does primary health care play in TB detection, prevention, and treatment?
Primary health care brings services closer to people, enabling early detection, timely diagnosis, prompt initiation of treatment, and continuous support throughout the course of care. It is also essential for contact tracing, reducing stigma, and working with communities to address the social determinants of the disease.
In other words, primary health care ensures that the response to tuberculosis is truly people-centered and accessible to all.
How does PAHO support countries in the prevention and elimination of tuberculosis?
Tuberculosis is among the diseases prioritized for elimination under the Elimination Initiative, and PAHO works with Member States to strengthen national responses through technical cooperation. This includes supporting the adoption of evidence-based recommendations, the implementation of new diagnostic and treatment tools, and the development of national capacities to improve surveillance and advance toward elimination.
In addition, through the PAHO Strategic Fund, countries can access quality medicines, supplies, and technologies at affordable prices, facilitating timely access to active case finding, diagnosis, and treatment. Examples include portable digital radiography equipment with artificial intelligence and molecular platforms for rapid TB diagnosis.
On World Tuberculosis Day, what message would you like to share with countries and communities in the Region?
Strengthened primary health care, with a fully integrated TB response, is essential to achieving TB elimination. This approach can expand access to more sensitive diagnostic tools and ensure that everyone, especially the most vulnerable, has access to timely, quality diagnosis and treatment.
At the same time, we must work with communities to reduce the stigma and discrimination associated with the disease. By placing people at the center of the response and making full use of available tools, it is possible to make sustained progress toward eliminating tuberculosis in the Region.




