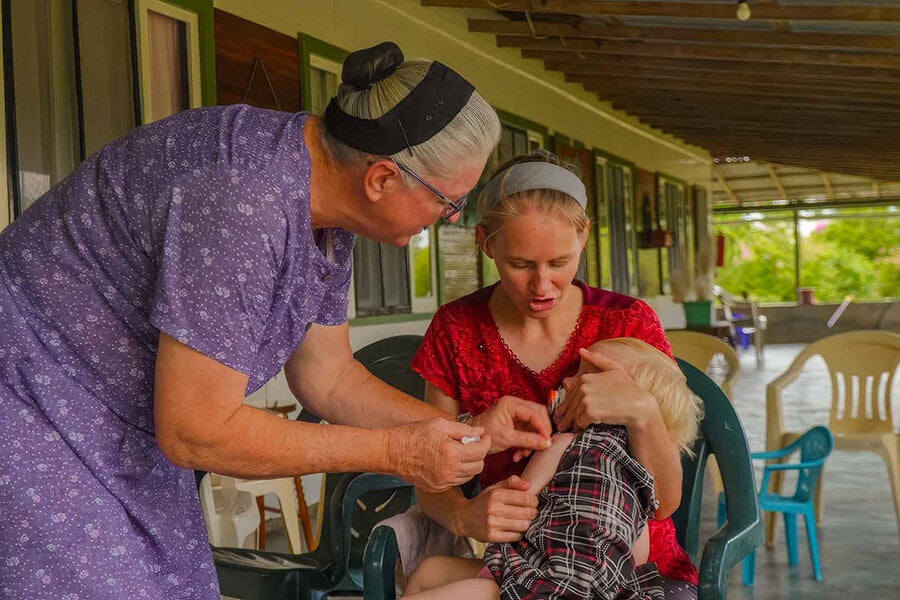
With technical support from the Pan American Health Organization and funding from the Government of Canada, Bolivia is strengthening vaccination efforts as the outbreak response continues.
— April 2026 —
After more than two decades without a locally transmitted case of measles, Bolivia has been facing an outbreak since 2025, which has spread across the country, from rural Mennonite colonies to isolated Indigenous communities. The response was immediate: mass vaccination, mobile health brigades, and active identification of people with incomplete vaccine schedules, even in the most isolated areas.
Across the country, the strategy combines science, community trust, and territorial presence. Vaccination remains the key to protecting lives.
Isidro Blatz, a Bolivian of Canadian descent, lives in the Mennonite colony of Belice. His family’s story traces the southern migration route, first settling in Mexico before deciding on Santa Cruz, Boliva. In these tight-knit communities, Mennonite families depend on agriculture, and dirt roads are still crossed by horse-drawn carts, suggesting a way of life that has changed little over time.
When he was 8, Isidro battled with measles. Nobody in his family was vaccinated. Fortunately, he survived, but the virus left invisible consequences and a lesson that would eventually fade.
In June 2025, measles returned to his life. His children, also unvaccinated, contracted the disease. They were not the only ones. Within weeks, entire families in Belice and those of other colonies, fell ill.