Throughout its 120 years of existence, PAHO has played a leading role in the response to epidemics in the region, including HIV/AIDS. Here are some of the important milestones, as well as the challenges that must be overcome to end AIDS.
August, 2022
Aaron Zea is 32 years old, a manager in the cultural sector, a cyclist who plays soccer every week and lives with HIV. "For me living with HIV is very peaceful because I know that I can have a normal life, play sports and go to university. I’m not going to die from this,” said Aaron, speaking from his home in Medellín, Colombia. In nine years of living with the virus, he knows what he needs to do to stay healthy - "look after my body, eat well, go to my check-ups and take my medications".
Today, treatment for HIV is effective and simple and generally consists of a single pill a day, with little to no adverse effects. However, this was not the case for people infected with HIV when Aaron was born in 1990, let alone in 1981, when the first cases of atypical pneumonia were diagnosed in gay men in San Francisco in the United States - something that would forever mark the lives of mankind.
New treatments have turned HIV infection into a chronic disease, and reduced mortality by 28% since 2010 in Latin America. However, this reduction remains below the global average due to huge advances in prevention, early detection, and the rapid initiation of treatment in Africa.
Today, 2.5 million people in Latin America and the Caribbean are living with HIV. Every year, around 120,000 people acquire the virus and some 35,000 lose their lives from AIDS-related causes, such as tuberculosis, cryptococcal meningitis, histoplasmosis or toxoplasmosis. Since 2010, the number of new infections has increased by 5% in Latin America, with a partial reduction in the Caribbean.
If a person who receives treatment manages to suppress the circulation of the virus in the blood, and does not transmit the infection, this is known as I = I or undetectable equals untransmissible, a powerful weapon of protection and prevention.
The first steps towards tackling a new epidemic
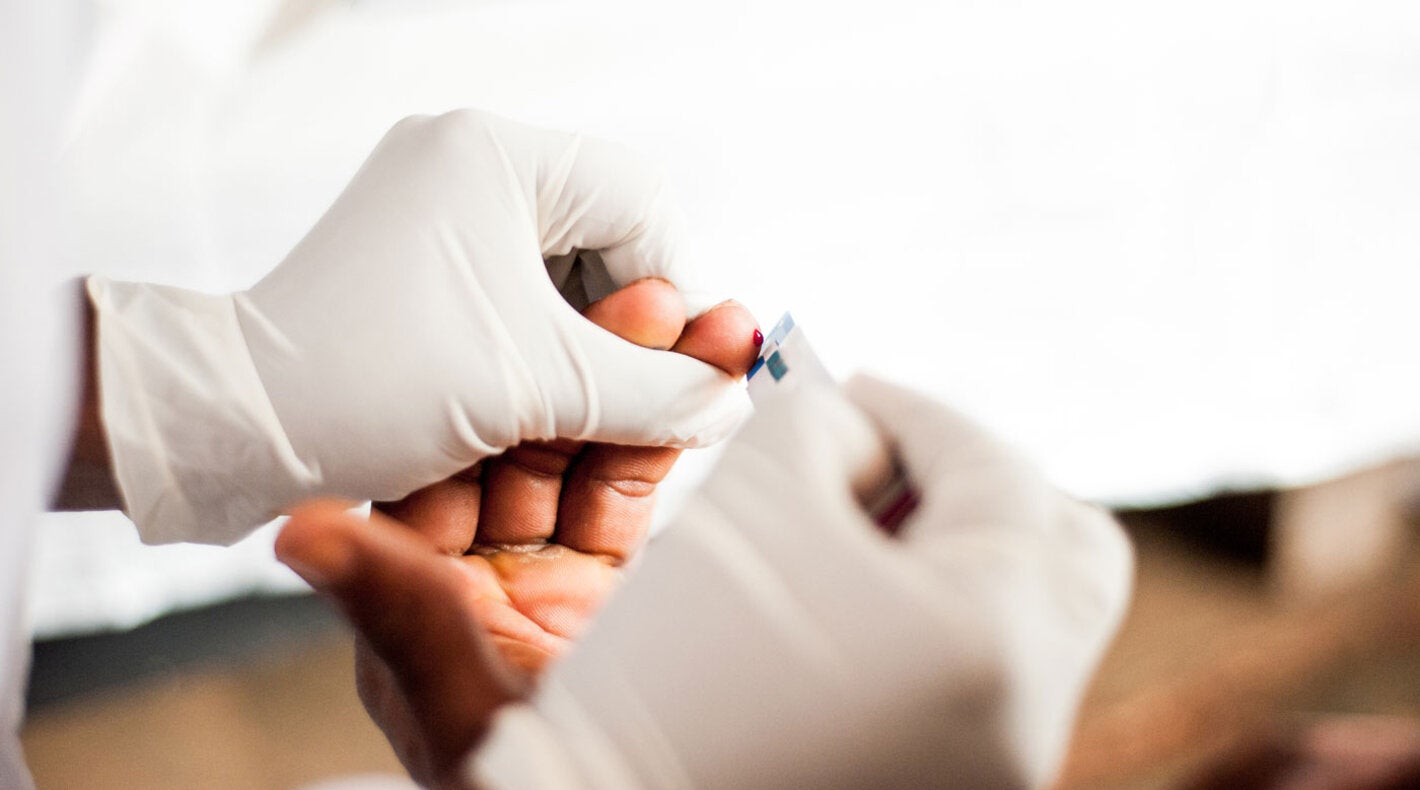
In 1984, three years after the first cases were detected, the Human Immunodeficiency Virus (HIV) was identified as the causative agent of AIDS, and the routes of transmission through blood, sexual relations and from mother to child were determined. The first test to diagnose the virus was developed in 1985.
The death of movie actor Rock Hudson from AIDS that year brought the issue to the attention of the world’s media and testing began en masse. However, with no antiretrovirals available, doctors could only treat the secondary infections. "Patients were slipping through our fingers," says infectologist Pedro Cahn, who worked at the Fernandez Hospital in Buenos Aires, Argentina, when the first cases appeared four decades ago.
Dr. Fernando Zacarías experienced the epidemic from the beginning. First, from the Centers for Disease Control and Prevention (CDC) in the United States and then as the first coordinator of the AIDS and Sexually Transmitted Diseases Program of the Pan American Health Organization (PAHO), in 1984.
"PAHO very quickly became alert to what was happening and was the first international health organization to address this problem," he says. "We adapted information from the U.S. National Institutes of Health and the CDC and disseminated the first guidelines for the region on how to prepare for the epidemic."
With resources from WHO's Special Program on AIDS, officially created in February 1987, PAHO sent teams of experts to countries in Latin American and the Caribbean to help them prepare their first action plans and establish national HIV/AIDS prevention and control programs.
PAHO also trained laboratories in the region to introduce testing, and supported campaigns to promote the use of condoms. Countries also began to introduce screening in blood banks to prevent HIV transmission, which had affected hemophiliacs at the beginning of the epidemic.
Activist pressure played a key role in reducing approval times for new drugs in the United States, and in 1987 AZT, the first antiretroviral against AIDS, was introduced.
The road to treatment for all
Until the first half of the 1990s, the drugs available to treat HIV were not effective in controlling the virus. Their cost was prohibitive for many (around US$400 per month), and public health programs continued to focus on prevention and treatment of the various secondary infections affecting AIDS patients.
Brazil and Argentina were the first countries in Latin America to provide free treatment. But this did not happen immediately in the rest of the countries in the region. However, thanks to the work of activists, and individuals that pursued legal action, many other governments soon began to provide the drugs free of charge through their public health programs.
During the World AIDS Conference in Vancouver, Canada, in 1996, a highly active antiretroviral therapy, or “cocktail”, was presented. This marked a turning point in treatment, making it possible to prevent the virus from replicating, recover CD4 lymphocytes that fight infection, reduce hospitalizations and improve survival.
Improving access to antiretrovirals
In order to support countries in improving access to essential medicines and medical supplies, PAHO created the Strategic Fund in 2000, a cooperation mechanism that helped ministries of health to acquire quality antiretrovirals at a lower and more affordable cost, plan for their demand and avoid stock-outs.
"In the past five years, the Strategic Fund has procured more than US$200 million in antiretrovirals, representing 2.5 million treatments for 22 countries in the Americas, as well as around 12 million diagnostic tests," said Christopher Lim, Head of the Strategic Fund. The Fund has also negotiated "reductions of up to 50% in the price of WHO-recommended treatments since 2017, representing savings of around US$20 million for PAHO Member States," he added.
Globally, most people under treatment currently receive the WHO-recommended preferred scheme, which consists of one pill a day combining the drugs tenofovir, lamivudine and dolutegravir (TLD). This is more effective, easier to take, has fewer side effects and can be used by almost everyone. It is also less prone to the emergence of treatment resistance and has better viral suppression rates.
In the Americas, 69% of people with HIV are on antiretroviral treatment, while the remainder are unaware of their status, or do not begin or continue treatment. The goal for 2030 is to diagnose at least 95% of all HIV-positive individuals, provide antiretroviral therapy for 95% of those diagnosed and achieve viral suppression for 95% of those treated.
"Latin America and the Caribbean have been at the forefront of an unprecedented response to HIV, once reaching the highest coverage of antiretroviral treatment in the world," says Dr. Rubén Mayorga, Head of HIV, Tuberculosis, Hepatitis and Sexually Transmitted Infections at PAHO. "However, today we are falling behind and must step up our response.”
Diagnosis, prevention, stigma and discrimination
In Latin America and the Caribbean, 2 out of 10 people with HIV do not know they are infected and 30% of people are diagnosed late, when their defenses are low and their lives are at risk.
"If we do not make access to testing universal, universal treatment is a fantasy because only those who know they have HIV can be treated," says Dr. Pedro Cahn. “This is why it is vital to normalize diagnosis and offer it as part of any medical consultation”.
The condom, which was the protagonist of hundreds of prevention campaigns in the 90s, is no longer the only prevention tool. Pre-exposure prophylaxis or PrEP, which consists of a pill with high efficacy to prevent infection, has been recommended since 2015 as an additional prevention option for those at substantial risk of becoming infected. Gay men and men who have sex with men, trans women, and female sex workers and their partners account for more than 90% of new cases in Latin America, so efforts must be prioritized to target these groups.
Stigma, discrimination and fear continue to keep many away from diagnosis and care and are another barrier that must be overcome to end AIDS as a public health problem by 2030 as proposed by the United Nations.
Accelerating the pace is also a crucial of ending this four-decade-old epidemic. "We have the tools to diagnose ourselves at home in 15 minutes, there are very effective and affordable treatments that enable people to live with the virus and not infect others, and anyone at substantial risk can now receive a pill that is around 99% effective in preventing infection when taken as prescribed. With all this, ending AIDS is possible," said Dr. Mayorga.