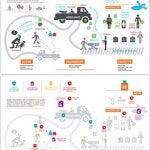
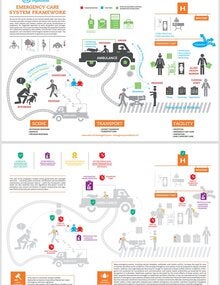
Timely and quality emergency care can make the difference between life and death. In the Region of the Americas, thousands of people face critical situations every day that require Emergency Care Systems (ECS) that are better prepared, coordinated, and accessible to all.
An ECS is an organized network of teams, supplies, functions, and health professionals that works in a coordinated and integrated manner to respond to life-threatening situations. This system includes prehospital care (care at the scene of the incident, transport, and transfer), care provided in health facilities (from primary care services to critical and surgical care units), as well as preparedness mechanisms and institutional safety measures for emergencies.
Strengthening the ECS is essential for all critical conditions, but it is particularly relevant in post-crash care, where a rapid, coordinated, and effective response can prevent avoidable deaths and reduce disabilities resulting from road traffic incidents.
The ECS not only seeks to provide clinical care but also to ensure that every person receives appropriate care in the right place and at the right time, through an organization that integrates governance, financing, information systems, and continuous quality improvement.
Through the Pan American Health Organization (PAHO), with the support of the United Nations Road Safety Fund (UNRSF) and other strategic partners, we are advancing an agenda to strengthen emergency care systems, with a focus on post-crash response, based on the essential components of the Emergency Care Systems Framework.
- The most recent data were published in Saving lives by promoting a safe systems approach to road safety in the Americas.
- Policy and governance:
- Six countries have a universal access provision law that mandates financial protection or requires free emergency care.
- Seventeen countries have a national law requiring health care facilities to provide care to any person experiencing an emergency.
- Canada, the United States, and Panama have a national Good Samaritan law.
- Thirteen countries report having a single national emergency access number with nationwide coverage.
- Fifteen countries reported including a response-time target in their road safety strategies; however, only Chile and Mexico included a response-time target defined in minutes.
- Twenty-five countries have an office, agency, or leading unit within the Ministry of Health or another ministry responsible for emergency care.
- Thirteen countries have a single emergency access number with nationwide coverage.
- National assessment (as of February 2026):
- Seven countries (Belize, Bolivia, Costa Rica, Guatemala, Jamaica, Paraguay, and Trinidad and Tobago) completed the Emergency and Critical Care System Assessment (ECCSA).
- Capacity strengthening (as of January 2026):
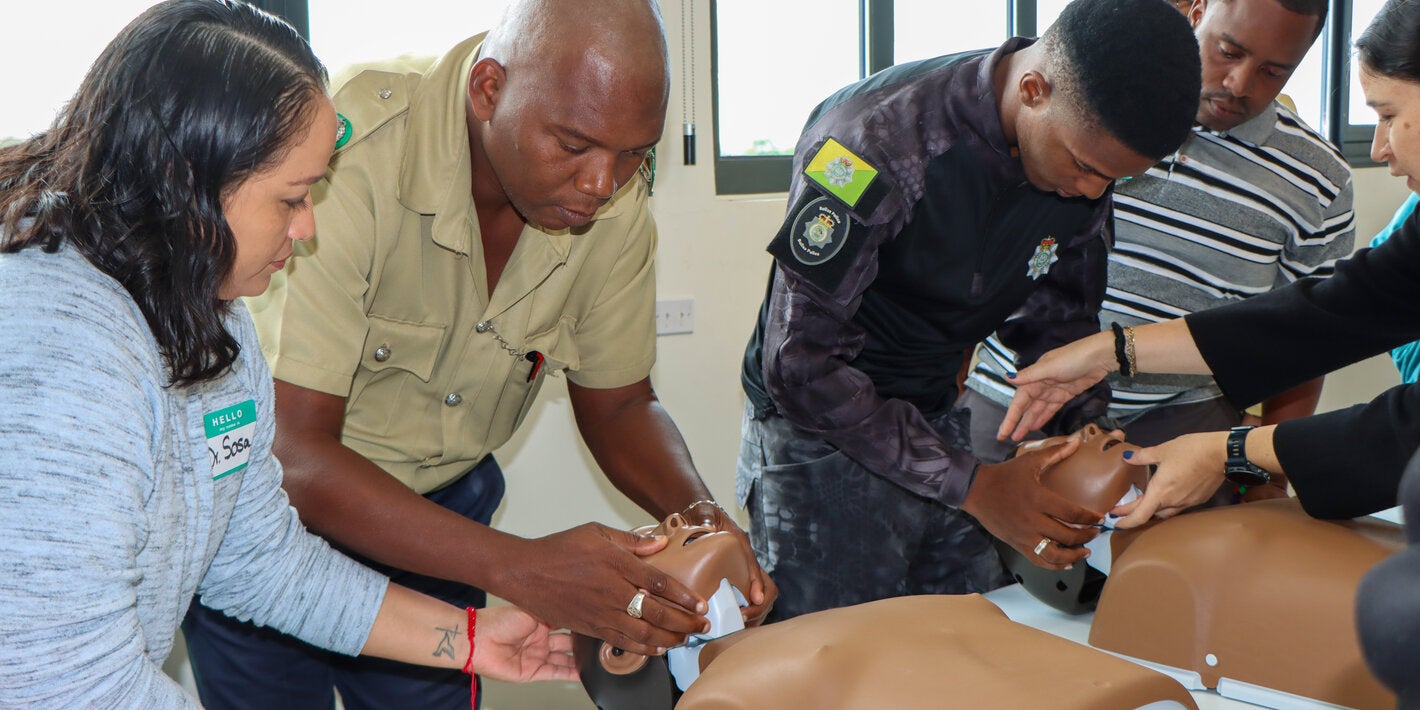
- Seven countries (Argentina, Bolivia, Colombia, Costa Rica, Jamaica, Mexico, and Paraguay) have implemented the cascade training program for the Basic Emergency Care (BEC) course.
- A total of 671 health professionals have been certified as BEC providers, and 182 facilitators have been trained to replicate the course in their respective countries.
- Belize implemented the Basic Critical Care (BCC) course.
- Costa Rica was the first country to implement the pilot phase of the Community First Aid Responder (CFAR) course. A total of 183 people have been trained in CFAR: 119 in Costa Rica and 64 police officers in Belize.
International commitment to the integration of emergency, critical, and surgical care has strengthened in recent years.
World Health Assembly resolution WHA76.2 (2023) highlighted the need to integrate emergency, critical, and surgical care services within health systems as key elements of universal health coverage and emergency preparedness. That same year, the United Nations General Assembly adopted resolution A/RES/78/4, reaffirming countries’ commitment to ensuring equitable access to essential health services.
In 2024, resolution WHA77.8 requested the development of a global strategy for 2026–2035 to integrate surgical, critical, and emergency care. In the Region of the Americas, these mandates are reflected in resolution CD61.R11 (2024), which approved the Integration Strategy 2025–2030, aimed at strengthening Emergency Care Systems at all levels of care. This strategy guides joint work with countries to build more resilient, equitable, and emergency-ready health systems.
PAHO works alongside countries in the Region of the Americas to strengthen emergency response capacity by promoting coordinated actions that save lives. These actions include the deployment of technical cooperation, the training of health professionals, the generation of evidence for decision-making, and the promotion of reforms that improve the preparedness and safety of Emergency Care Systems.