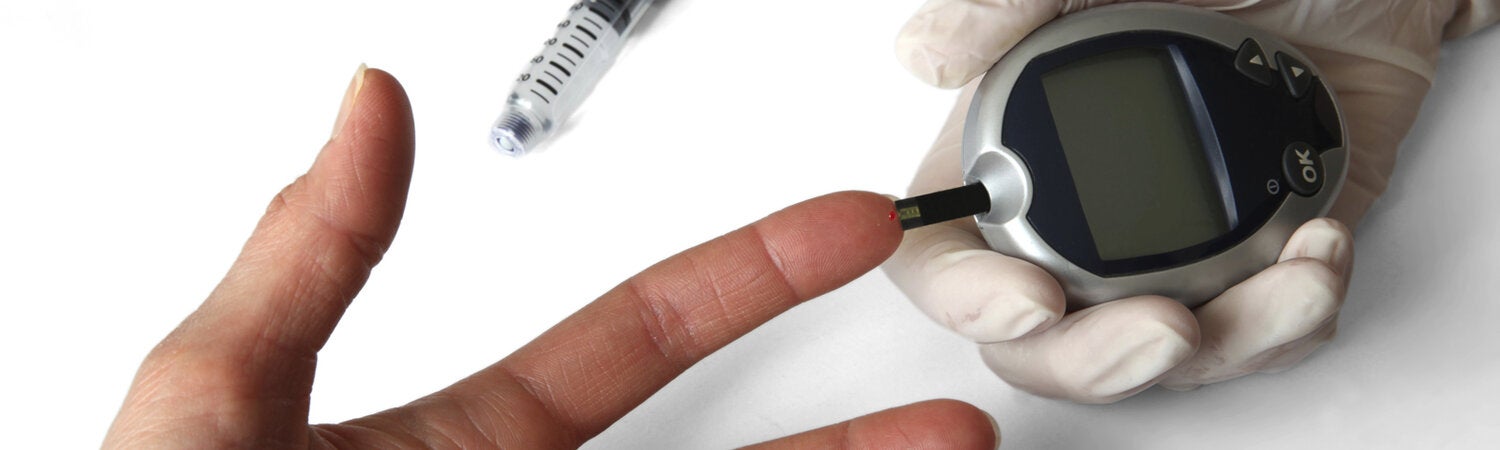
Diabetes is a chronic, metabolic disease characterized by elevated levels of blood glucose (or blood sugar), which leads over time to serious damage to the heart, blood vessels, eyes, kidneys, and nerves. The most common is type 2 diabetes, usually in adults, which occurs when the body becomes resistant to insulin or doesn't make enough insulin. In the past three decades, the prevalence of type 2 diabetes has risen dramatically in countries of all income levels. Type 1 diabetes, once known as juvenile diabetes or insulin-dependent diabetes, is a chronic condition in which the pancreas produces little or no insulin by itself. For people living with diabetes, access to affordable treatment, including insulin, is critical to their survival. There is a globally agreed target to halt the rise in diabetes and obesity by 2025
Symptoms of type 1 diabetes include the need to urinate often, thirst, constant hunger, weight loss, vision changes, and fatigue. These symptoms may occur suddenly.
Symptoms of type 2 diabetes are generally similar to those of type 1 diabetes but are often less marked. As a result, the disease may be diagnosed several years after onset, by which time complications have already arisen. For this reason, it is important to be aware of risk factors.
Although type 1 diabetes cannot currently be prevented, effective approaches are available to prevent type 2 diabetes and the complications and premature death that can result from all types of diabetes. These include policies and practices across whole populations and within specific settings (school, home, workplace) that contribute to good health for everyone, regardless of whether they have diabetes, such as exercising regularly, eating healthily, avoiding smoking, and controlling blood pressure and lipids.
The starting point for living well with diabetes is an early diagnosis—the longer a person lives with undiagnosed and untreated diabetes, the worse their health outcomes are likely to be. Therefore, easy access to basic diagnostics, such as blood glucose testing, should be available in primary healthcare settings. Patients will need periodic specialist assessment or treatment for complications.
A series of cost-effective interventions can improve patient outcomes, regardless of the type of diabetes. These interventions include blood glucose control through a combination of diet, physical activity, and, if necessary, medication; control of blood pressure and lipids to reduce cardiovascular risk and other complications; and Prevention and treatment.
- 112 million adults (18 years or older) live with Diabetes in the Americas, a number that has tripled in the Region since 1990. Prevalence has been rising more rapidly in low—and middle-income countries than in high-income countries.
- Diabetes is a major cause of blindness, kidney failure, heart attacks, stroke, and lower limb amputation. Poorly controlled diabetes increases the chances of these complications and premature mortality. In addition, people with diabetes are at higher risk of presenting cardiovascular diseases and tuberculosis, especially those with poor glycemic control.
- The burden of disease associated with diabetes is enormous and growing: in just 20 years, diabetes mortality has increased by over 50% worldwide. In the Region of the Americas, it is the sixth leading cause of death and the fifth cause of years of life lost prematurely.
- In the Region, diabetes (including diabetes-related kidney disease) causes approximately eight million years of life lost each year due to premature death.
- Diabetes is currently the third cause of DALYs, preceded only by ischemic heart disease and COVID-19.
- The expansive increase in the diabetes epidemic goes hand in hand with the increase in its risk factors. The Americas is the region with the most overweight/obesity and physical inactivity in the world: 68 out of every 100 adults are overweight or obese, and 36 out of every 100 people have an insufficient level of physical activity.
- The increase in risk factors for type 2 diabetes is alarming in children and adolescents. 16 out of 100 adolescents and 19 out of 100 children are obese, while 81 out of 100 adolescents do not engage in enough physical activity.
- Diabetes can be treated and its consequences avoided or delayed with diet, physical activity, medication, and regular screening and treatment for complications.
Type 1 Diabetes
Type 1 diabetes (previously known as insulin-dependent, juvenile or childhood-onset) is characterized by deficient insulin production and requires daily administration of insulin. In 2017 there were 9 million people with type 1 diabetes; the majority of them live in high-income countries. Neither its cause nor the means to prevent it are known.
Symptoms include excessive excretion of urine (polyuria), thirst (polydipsia), constant hunger, weight loss, vision changes, and fatigue. These symptoms may occur suddenly.
Type 2 Diabetes
Type 2 diabetes (formerly called non-insulin-dependent, or adult-onset) results from the body’s ineffective use of insulin. More than 95% of people with diabetes have type 2 diabetes. This type of diabetes is largely the result of excess body weight and physical inactivity.
Symptoms may be similar to those of type 1 diabetes but are often less marked. As a result, the disease may be diagnosed several years after onset, after complications have already arisen.
Until recently, this type of diabetes was seen only in adults but it is now also occurring increasingly frequently in children.
Gestational Diabetes
Gestational diabetes is hyperglycaemia with blood glucose values above normal but below those diagnostic of diabetes. Gestational diabetes occurs during pregnancy.
Women with gestational diabetes are at an increased risk of complications during pregnancy and at delivery. These women and possibly their children are also at increased risk of type 2 diabetes in the future.
Gestational diabetes is diagnosed through prenatal screening, rather than through reported symptoms.
Impaired glucose tolerance and impaired fasting glycaemia
Impaired glucose tolerance (IGT) and impaired fasting glycaemia (IFG) are intermediate conditions in the transition between normality and diabetes. People with IGT or IFG are at high risk of progressing to type 2 diabetes, although this is not inevitable.
Health impact
Over time, diabetes can damage the heart, blood vessels, eyes, kidneys, and nerves.
- Adults with diabetes have a two- to three-fold increased risk of heart attacks and strokes(1).
- Combined with reduced blood flow, neuropathy (nerve damage) in the feet increases the chance of foot ulcers, infection and eventual need for limb amputation.
- Diabetic retinopathy is an important cause of blindness, and occurs as a result of long-term accumulated damage to the small blood vessels in the retina. Close to 1 million people are blind due to diabetes(2).
- Diabetes is among the leading causes of kidney failure(3).
Prevention
Simple lifestyle measures have been shown to be effective in preventing or delaying the onset of type 2 diabetes. To help prevent type 2 diabetes and its complications, people should:
- achieve and maintain a healthy body weight;
- be physically active – doing at least 30 minutes of regular, moderate-intensity activity on most days. More activity is required for weight control;
- eat a healthy diet, avoiding sugar and saturated fats; and
- avoid tobacco use – smoking increases the risk of diabetes and cardiovascular disease.
Diagnosis and treatment
Early diagnosis can be accomplished through relatively inexpensive testing of blood sugar.
Treatment of diabetes involves diet and physical activity along with lowering of blood glucose and the levels of other known risk factors that damage blood vessels. Tobacco use cessation is also important to avoid complications.
Interventions that are both cost-saving and feasible in low- and middle-income countries include:
- blood glucose control, particularly in type 1 diabetes. People with type 1 diabetes require insulin, people with type 2 diabetes can be treated with oral medication, but may also require insulin;
- blood pressure control; and
- foot care (patient self-care by maintaining foot hygiene; wearing appropriate footwear; seeking professional care for ulcer management; and regular examination of feet by health professionals).
Other cost saving interventions include:
- screening and treatment for retinopathy (which causes blindness);
- blood lipid control (to regulate cholesterol levels);
- screening for early signs of diabetes-related kidney disease and treatment.
PAHO/WHO aims to stimulate and support the adoption of effective measures for the surveillance, prevention and control of diabetes and its complications, particularly in low- and middle-income countries. To this end, PAHO/WHO:
- provides scientific guidelines for the prevention of major noncommunicable diseases including diabetes;
- develops norms and standards for diabetes diagnosis and care;
- builds awareness on the global epidemic of diabetes, marking World Diabetes Day (14 November); and
- conducts surveillance of diabetes and its risk factors.
The WHO Global report on diabetes provides an overview of the diabetes burden, interventions available to prevent and manage diabetes, and recommendations for governments, individuals, the civil society and the private sector.
The WHO module on diagnosis and management of type 2 diabetes brings together guidance on diagnosis, classification and management of type 2 diabetes in one document. The module is for policy-makers who plan service delivery of diabetes care, national programme managers responsible for training, planning and monitoring service delivery, and facility managers and primary care staff involved in clinical care and monitoring processes and outcomes of diabetes care.
In April 2021 WHO launched the Global Diabetes Compact, a global initiative aiming for sustained improvements in diabetes prevention and care, with a particular focus on supporting low- and middle-income countries. The Compact is bringing together national governments, UN organizations, nongovernmental organizations, private sector entities, academic institutions, and philanthropic foundations, people living with diabetes, and international donors to work on a shared vision of reducing the risk of diabetes and ensuring that all people who are diagnosed with diabetes have access to equitable, comprehensive, affordable and quality treatment and care.
In May 2021, the World Health Assembly agreed a Resolution on strengthening prevention and control of diabetes. It recommends action in areas including increasing access to insulin; promoting convergence and harmonization of regulatory requirements for insulin and other medicines and health products for the treatment of diabetes; and assessing the feasibility and potential value of establishing a web-based tool to share information relevant to the transparency of markets for diabetes medicines and health products.
We're committed to improving diabetes care through the Better Care for NCDs initiative. Discover how we're transforming the approach to NCDs in primary health care.