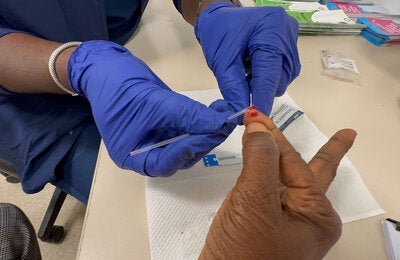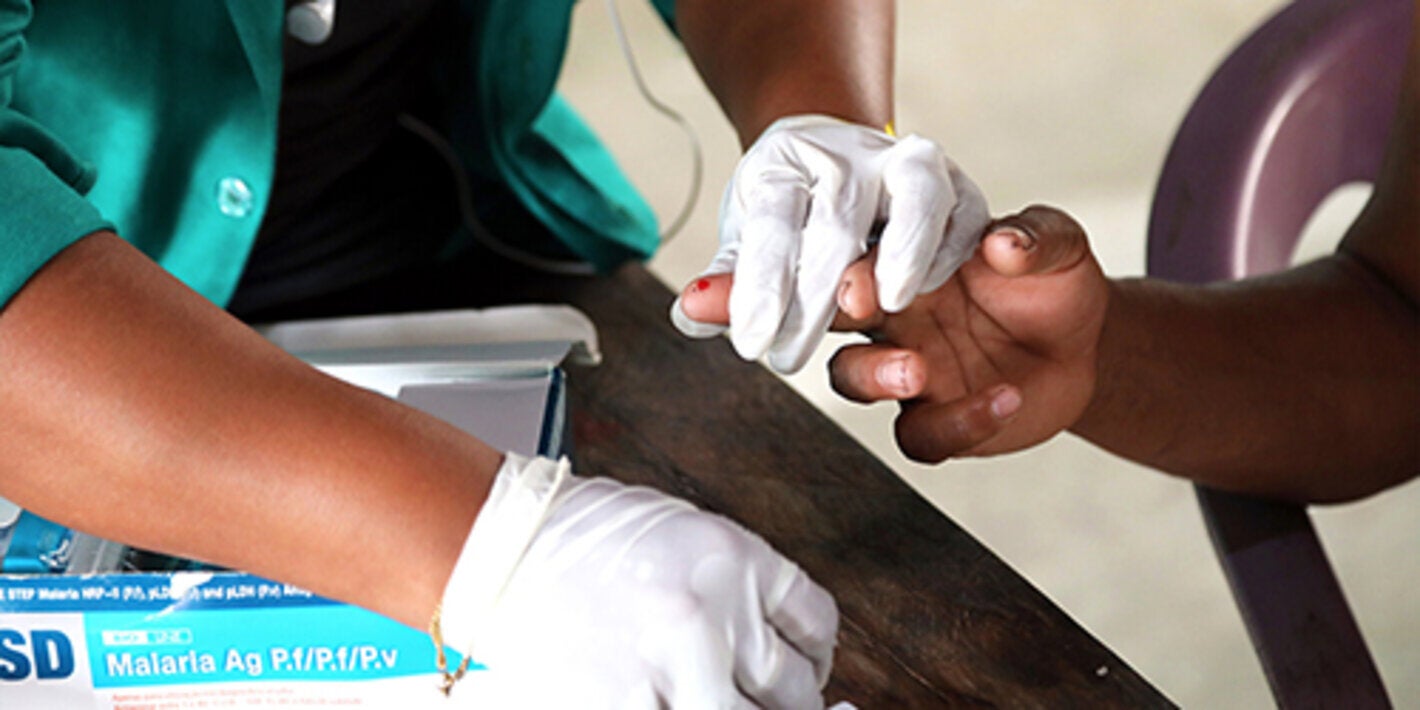
Countries must balance COVID-19 response with maintaining essential services to manage and prevent infectious diseases.
Washington, D.C., Aug. 11, 2020 (PAHO)— The pandemic of COVID-19, which has killed over 390,000 people in the Americas, is threatening regional plans to eliminate and control infectious diseases including tuberculosis, HIV, hepatitis and others, PAHO Director Carissa F. Etienne said today.
With more than 10.5 million cases of COVID-19 in the Americas and 100,000 new cases being reported every day, “countries can’t delay the fight against COVID-19, but we must not let COVID-19 delay us in completing our unfinished agenda of eliminating and controlling infectious diseases from our region,” she told a press briefing.
Challenges in delivering TB treatments during the pandemic were reported by 80 percent of the countries in Latin America and the Caribbean, which could turn manageable cases of TB into active infections. Similarly, 30 percent of people living with HIV are avoiding seeking care and antiretroviral medications are in limited supply. Disruptions in hepatitis screenings, key for detection and treatment, were also reported by a third of the countries.
The PAHO Director recalled that preventing and treating infectious diseases was the impetus for creating the Pan American Health Organization nearly 120 years ago and the Region remains “at the forefront of the elimination of infectious diseases.”
Indeed, in October 2019, PAHO’s Member States committed to a region-wide approach to the elimination of more than 30 communicable diseases and related conditions in the Americas by 2030.
But “The progress to achieving this milestone is now under threat, due to the burden of COVID-19 on health systems, and the disruption of essential services, including priority disease control programs, elimination initiatives and routine immunization,” the PAHO director noted.
The pandemic also interrupted mass drug administration campaigns that are vital to elimination efforts “just as we were making significant progress against neglected tropical diseases, like lymphatic filariasis, schistosomiasis, and soil-transmitted helminthiases,” she said.
Dengue and malaria remain a huge burden on health services and, like COVID-19, have a disproportionate impact on poor and vulnerable populations, including indigenous communities, she said.
PAHO’s director said “In the first two months of 2020 the Americas reported a 139% increase in dengue cases when compared to the same period in 2019. However, since COVID-19 hit our region in March, reported cases of dengue fever have actually fallen.”
Reporting of mosquito borne diseases, like malaria, “is down more than 40%, and there has been an observed reduction in the number of people getting tested. So we know that these data don’t tell the full story,” she said.
“While it is true that because many of us are stuck at home we’re less prone to getting bitten by mosquitoes, the reality is that mosquitoes and the pathogens they transmit are still circulating. And without testing or treatment, severe cases of mosquito-borne diseases could go from easily treatable conditions to death,” Dr. Etienne noted.
She said health systems must make it easier for patients to receive care, by “leveraging telemedicine and offering care outside of hospital settings, such as via community outreach programs and at-home visits.”
They also need to protect health workers on the front lines of this pandemic. “Our doctors, nurses and staff must have the protective equipment, supplies and technologies they need to safely offer care” so patients can continue to receive the medical attention and the medications they need to safely manage their conditions, she said.
Contacts
Leticia Linn
Sebastian Oliel
Ashley Baldwin
mediateam@paho.org