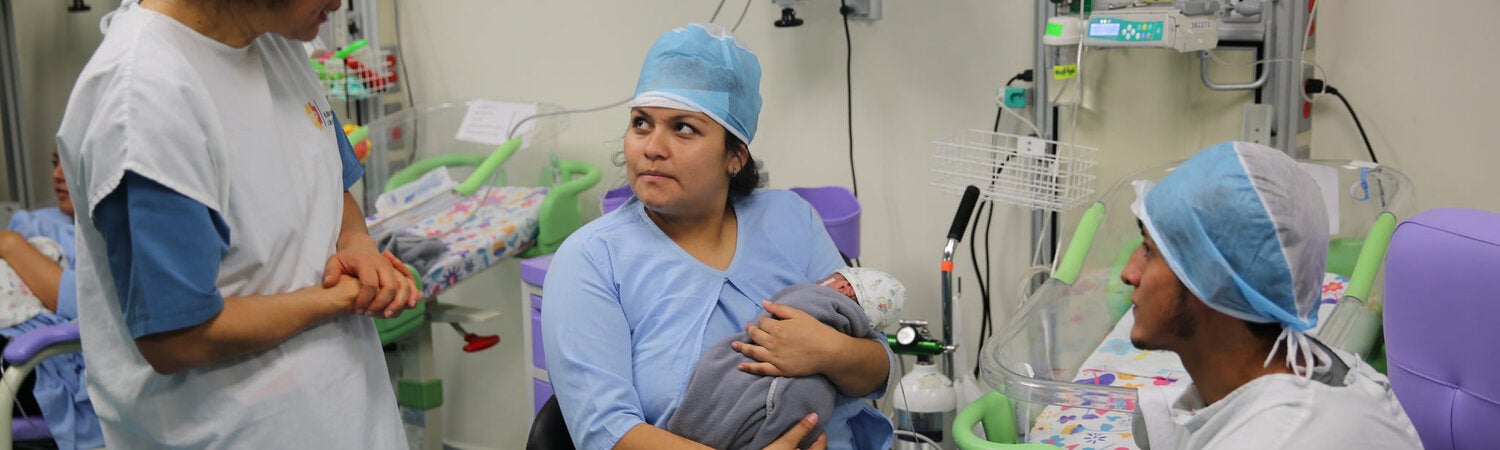
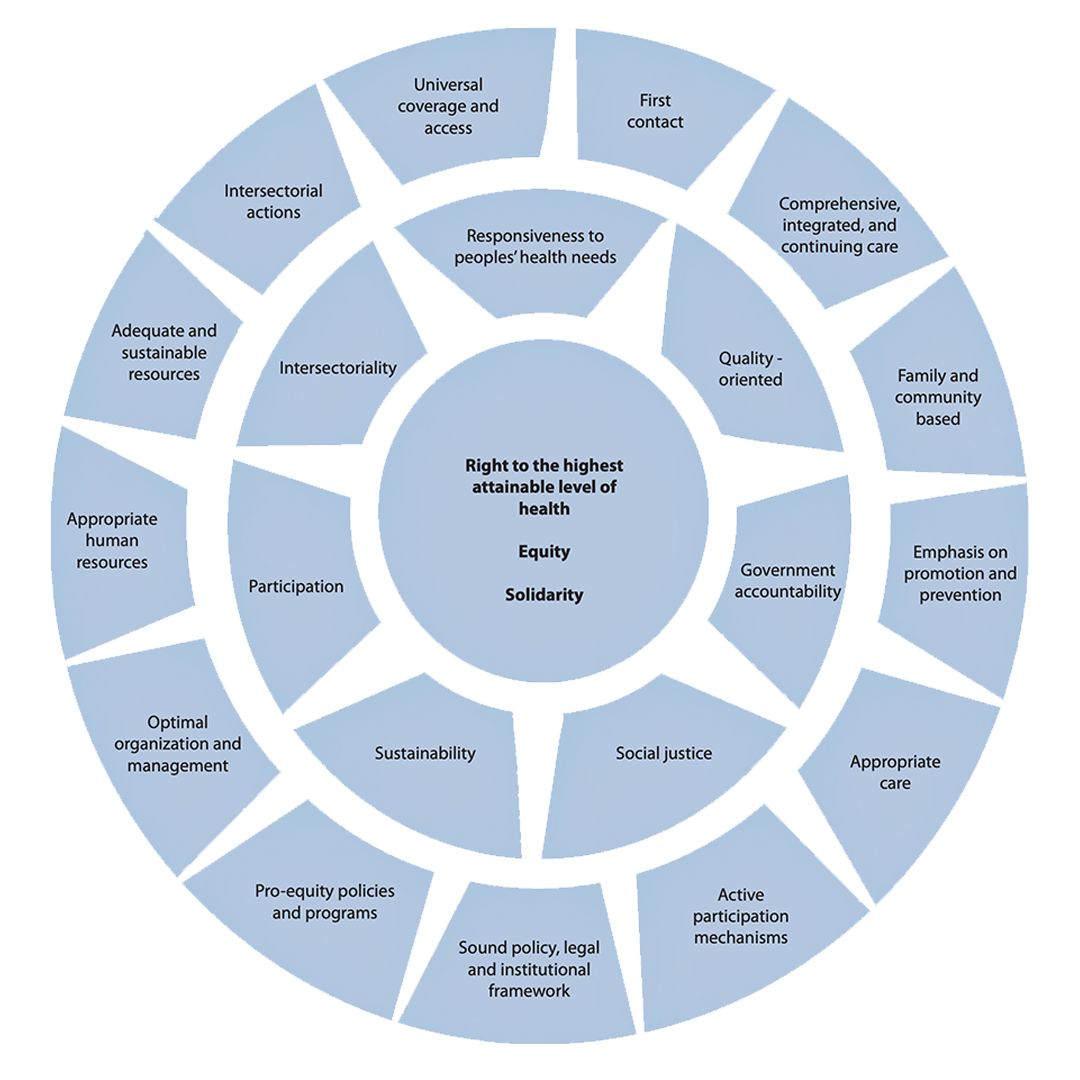
PAHO considers Integrated health services networks as one of the principal operational expressions of Primary Health Care-based health systems at the health services level, helping to make several of its most essential elements a reality such as universal coverage and access, first contact,comprehensive, integrated and continuing care, appropriate care, optimal organization and management, family and community orientation, and intersectoral action, among others.
- The purpose of the PAHO Initiative on Integrated Health Service Delivery Networks (IHSDNs) is to contribute to the development of PHC-based health systems, and thus to health services delivery that is more accessible, equitable, efficient, of higher technical quality, and that better fulfills citizens’ expectations
- PAHO considers IHSDNs as one of the principal operational expressions of PHC-based health systems at the health services level, helping to make several of its most essential elements a reality such as universal coverage and access, first contact, comprehensive, integrated and continuing care, appropriate care, optimal organization and management, family and community orientation, and intersectoral action, among others
Fragmentation of health services is a major cause of poor performance of health services, and thus of the underperformance of health systems in general. Fragmentation can generate, on its own, or combined with other factors, difficulties in access to services, delivery of services of poor technical quality, irrational and inefficient use of available resources, unnecessary increases in production costs, and low user satisfaction with services received.
In response to the challenges posed by health services fragmentation and to various international mandates and commitments, PAHO/WHO is developing the initiative on Integrated Delivery Networks (IDN) with a view to contribute to the strengthening of Health Systems based on Primary Health Care (PHC), and thus to the delivery of more accessible, equitable, efficient, and quality health services that better meet the expectations of the population.