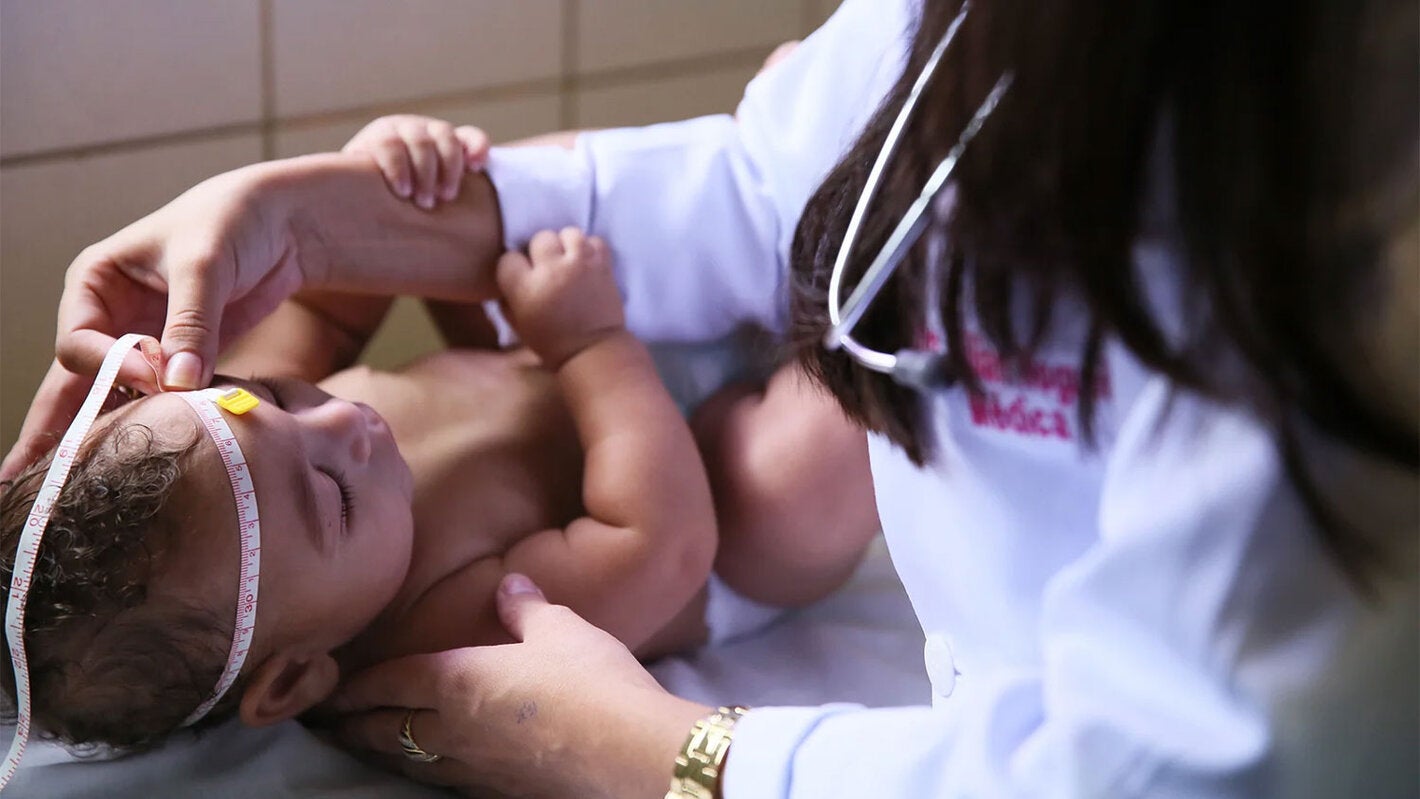
In 2015 and 2016, the word Zika evoked fear in pregnant women living or traveling to tropical areas of the Americas. In countries where the mosquito-borne disease spread, babies of some infected mothers were being born with microcephaly, marked by abnormally small heads, brain damage and a future of developmental problems.
October 2022
The Zika virus infection is caused by the bite of an infected Aedes aegypti mosquito, usually causing rash, mild fever, conjunctivitis, and muscle pain. One in four infected people develop symptoms and, among those who do, the disease is usually mild and can last 2-7 days.
But a new picture emerged in the State of Pernambuco in north-eastern Brazil in September 2015, when epidemiologists suspected that Zika could be behind a surge of babies born with microcephaly.
The virus was first isolated in 1947 in the Zika forest of Uganda, giving it its name. For decades, it remained mainly in Africa, with small and sporadic outbreaks in Asia.
In 2007, a major epidemic was reported on the island of Yap in Micronesia, where nearly 75% of the population was infected, and from there it appeared in Latin America, in a seemingly more virulent and harmful form.
As soon as the Pan American Health Organization (PAHO) and the Global Outbreak Alert and Response Network (GOARN) alerted Brazilian authorities of a highly probable association of Zika and microcephaly, PAHO declared an emergency on 5 December 2015 and started to help countries in the response. Subsequently, the World Health Organization (WHO) declared Zika a Public Health Emergency of International Concern on 1 February 2016, which would last until November 2016.
The challenge the virus would bring to the region was formidable: by the end of 2016, 48 countries and territories in the Americas had reported more than 532,000 suspected infections, including 175,063 confirmed cases. In addition, 22 countries and territories reported 2,439 cases of congenital syndrome associated with Zika, mostly in Brazil.
“The outbreak was a complicated chess game,” said Dr. Sylvain Aldighieri, the PAHO Incident Manager at the time of the Zika epidemic, “with many moving parts, all of which were constantly evolving, making it much more challenging for scientists to study and understand.”
The situation was especially worrying due to the sheer number of vulnerable populations. “Across PAHO member states, we have more than 500 million people living in areas at risk of Zika, Dengue, or Chikungunya, because of the presence of the Aedes Aegypti mosquito,” Dr. Aldighieri added.
PAHO’s “Three Pillar Strategy” as Zika spread in the region
As the Zika virus spread rapidly throughout the Americas, PAHO coordinated a regional response, deploying over 80 expert missions to help its Member States tackle the outbreak.
“The organization developed a comprehensive strategy based on three pillars: prevention, detection and response to help countries,” said Dr. Marcos Espinal, PAHO's interim Assistant Director, who was at that time Director of Communicable Diseases and Health Analysis at PAHO and an integral part of the Zika emergency response in 2016.
Central to the efforts was controlling the Zika vector, which included mosquito surveillance and recommendations for the elimination of mosquitoes’ breeding sites, such as uncovered containers and buckets.
Communicating the risk to affected populations and raising public awareness were key, recalled Dr. Espinal. PAHO supported countries in disseminating information about how to avoid mosquito-borne diseases, including Zika.
Another important element was issuing recommendations to all countries of the Americas for prenatal and postnatal care and guidelines for children affected by microcephaly, ranging from early stimulation to the type of tests and monitoring they should follow.
To achieve a swift response, PAHO worked alongside partners, such as the Centers for Disease Control and Prevention (CDC) and the Public Health Agency of Canada (PHAC), the Instituto de Medicina Tropical Pablo Kouri (IPK), the Oswaldo Cruz Foundation (Fiocruz), the Pasteur Institute International Network, and ministries of health from across Latin America, especially in Brazil.
Seven years on – Zika today
The scientific community is still learning about Zika and currently there is no specific medicine or vaccine to prevent an infection with the virus. Although there are some promising vaccines in the pipeline, the best prevention is still avoiding mosquito bites.
In 2022, PAHO reported nearly 30,000 cases throughout the Americas, and four deaths. To date, Brazil is the country with the highest cumulative incidence.
Although the virus is now circulating in low levels across the region, the 2016 outbreak had a lasting impact: the babies born with microcephaly during the 2015-2016 outbreak are now turning 6 and 7 years old. Their developmental challenges continue as parents and health authorities grapple with their condition. “It is important to not let our guard down. Surveillance efforts need to be maintained to ensure we can respond quickly when the virus is detected,” said Dr. Espinal.
Due to the pandemic, resources destined to tackle arboviral diseases like Zika were rerouted to deal with the heavy demand for medical care brought by COVID-19, pushing back the clock on Zika research and development.
“Zika is still a public health challenge, and we must remain vigilant. Ongoing research is vital – as we understand more about how the Zika virus works and affects cells, we can look forward to a day when scientists eventually find a much-needed vaccine or treatment,” said Dr. Aldighieri.
PAHO continues to help countries in developing and maintaining the ability to detect and confirm cases, treat people and implement effective strategies to reduce the presence of mosquitoes.