Respiratory viruses such as influenza, SARS-CoV-2, RSV, and others pose significant public health challenges worldwide. The Pan American Health Organization (PAHO) is supporting its Member States to detect, monitor, prevent, and control these infections across the Americas.
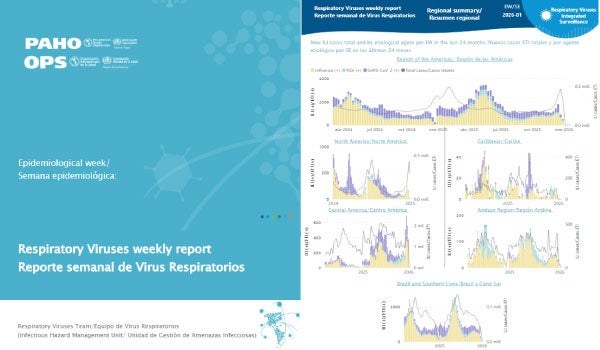
This page serves as a comprehensive resource, offering up-to-date information, surveillance data, guidelines, and technical resources for the general public and to support healthcare professionals, policymakers, and researchers. It also describes how PAHO collaborates with countries to strengthen their capacity to detect and respond to respiratory virus outbreaks, protecting the health of communities across the region.
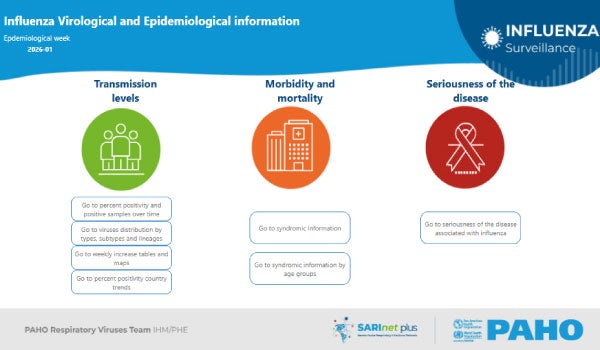
Seasonal influenza is an acute respiratory disease caused by influenza A and B viruses. It is mainly transmitted through respiratory droplets, aerosols in enclosed spaces, and contact with contaminated surfaces. Common signs and symptoms include fever, dry cough, sore throat, nasal congestion, headache, and muscle pain.
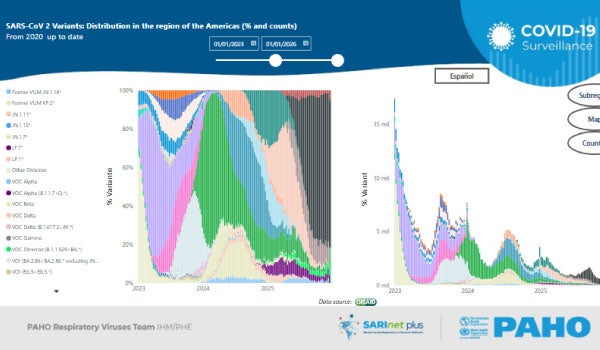
SARS-CoV-2 is the virus that causes COVID-19, a respiratory disease mainly transmitted through respiratory droplets, aerosols in enclosed spaces, and contact with contaminated surfaces. The most common symptoms include fever, cough, sore throat, nasal congestion, headache, respiratory distress, and loss of smell or taste.
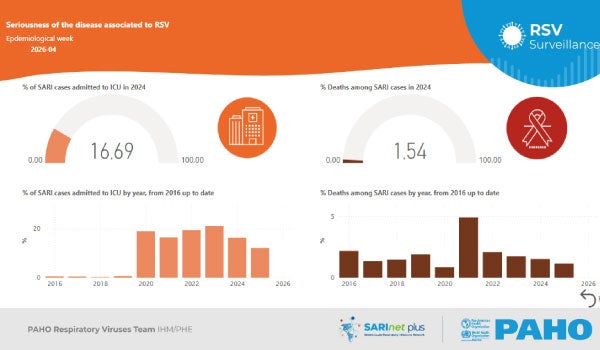
Respiratory syncytial virus (RSV) causes respiratory infections, particularly in infants and young children, and is mainly transmitted through respiratory droplets and contact with contaminated surfaces. The most common symptoms include cough, nasal congestion, sneezing, fever, wheezing, and respiratory distress.
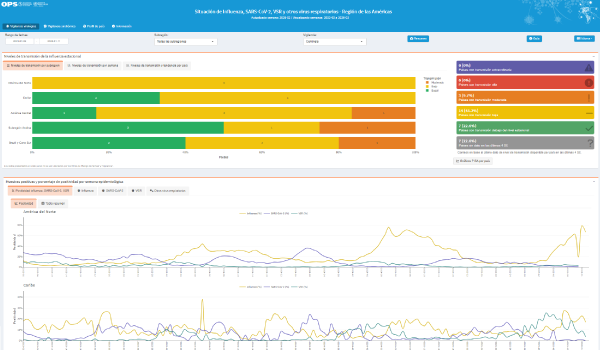
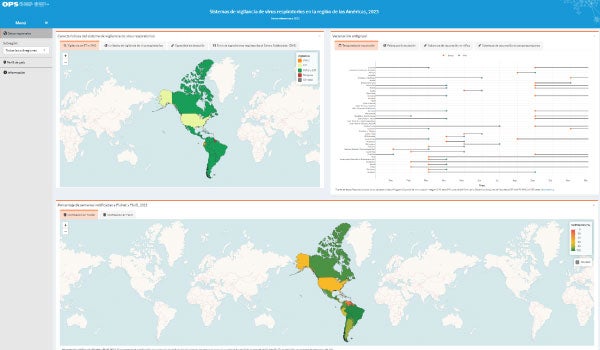
The organization supports countries in the surveillance, prevention, preparedness, and control of pandemic & epidemic-prone diseases through the development of evidence-based strategies to predict, prevent, detect, and respond to infectious hazards. It also ensures regional surveillance functions related to these hazards.
Major Action Lines:
- Pandemic & epidemic-prone diseases: Influenza, MERS, hemorrhagic fevers and hantavirus, yellow fever & emerging arboviruses, plague, cholera & epidemic-prone diarrheal diseases, leptospirosis, meningococcal disease.
- Expert networks and interventions for surveillance and response: epidemiology and modeling, laboratory, clinical management, and infection prevention & control.